Advanced Ultrasound in Diagnosis and Therapy ›› 2025, Vol. 9 ›› Issue (2): 207-214.doi: 10.37015/AUDT.2025.230059
• Original Research • Previous Articles Next Articles
Lin Jiaojiaoa,b,1, Ke Helina,1, Xu Shaodana, Xiao Yanga, Han Linaa, Lyu Guoronga,c,*( ), Li Shilina,*(
), Li Shilina,*( )
)
Received:2024-01-04
Revised:2023-12-06
Accepted:2024-09-05
Online:2025-06-30
Published:2025-07-06
Contact:
Address Department of Medicine, Quanzhou Medical College. No. 2 Anji Road, Luojiang District, Quanzhou, 362000, China (GRL).e-mail: About author:First author contact:1Jiaojiao Lin and Helin Ke contributed equally to this paper.
Lin Jiaojiao, Ke Helin, Xu Shaodan, Xiao Yang, Han Lina, Lyu Guorong, Li Shilin. Improved Ultrasound Evaluation Method for Diagnosing Nonalcoholic Fatty Pancreatic Disease: Correlation with MRI mDixon-Quant. Advanced Ultrasound in Diagnosis and Therapy, 2025, 9(2): 207-214.
Table 1
Improved ultrasonic diagnostic method nonalcoholic fatty pancreatic disease grading standards"
| Grade | Compared with echo of RC | Pancreas itself | Pancreatic duct | Pancreatic outline | SMA、PV |
|---|---|---|---|---|---|
| 0 | No difference | No enlargement | Visible | Smooth | Clearly visible |
| 1 | Mild Enhancement | No enlargement | Visible | Smooth | Clearly visible |
| 2 | Moderate enhancement | Enlargement | Blurred | Blurred | Blurred |
| 3 | Significant enhancement | Significant enlargement | Invisible | Invisible | Invisible |
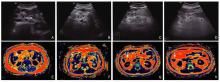
Figure 1
Improved ultrasound grading criteria for Nonalcoholic Fatty Pancreas Disease (NAFPD). (A-D) represent ultrasound images for NAFPD Grades 0 to 3, respectively, with pancreatic tissue (☆), retroperitoneal visceral fat (black arrow), and splenic vein (SV) annotated. (E-H) Corresponding magnetic resonance imaging (MRI) findings of abdominal fat distribution (white arrow) for NAFPD Grades 0-3."
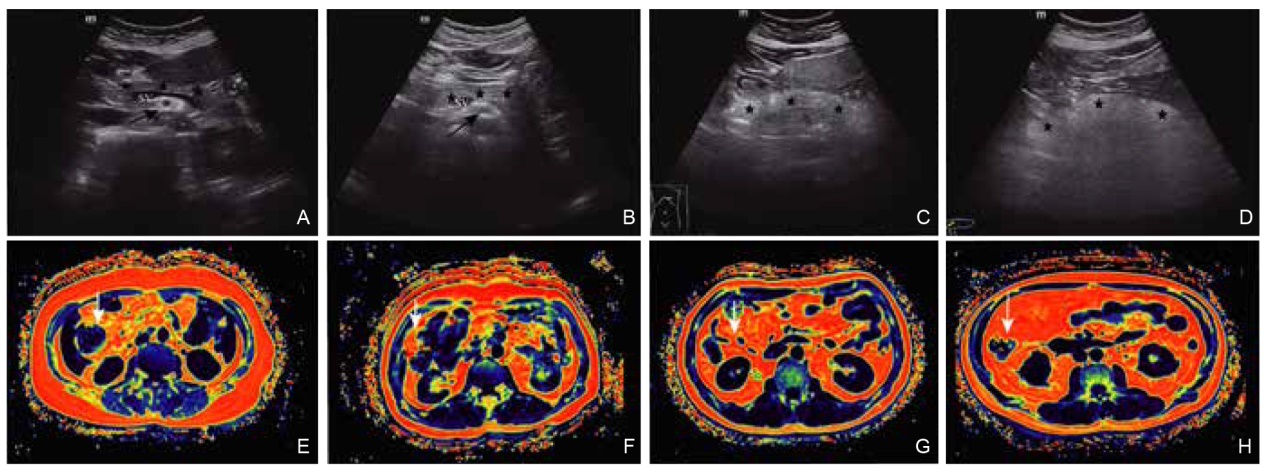
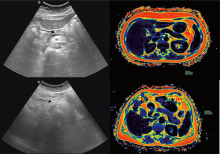
Figure 2
(A) A 54-year-old female US image, with a NAFPD score of grade 1; (B) mDixon-quant image of the same subject as in (A), showing a fat quantification of 0.54%; (C) A 52-year-old female US image, with a NAFPD score of grade 3; (D) mDixon-quant image of the same subject as in (C), showing a fat quantification of 11.84%. Arrow: Pancreas."
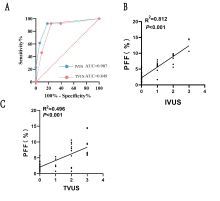
Figure 3
(A) Receiver operating characteristic curve of the traditional version of ultrasound and improved ultrasonic diagnostic method for the diagnosis of nonalcoholic fatty pancreatic disease; (B) and (C) Correlation between pancreatic fat fraction and grade as determined using two pancreatic ultrasound grading methods."
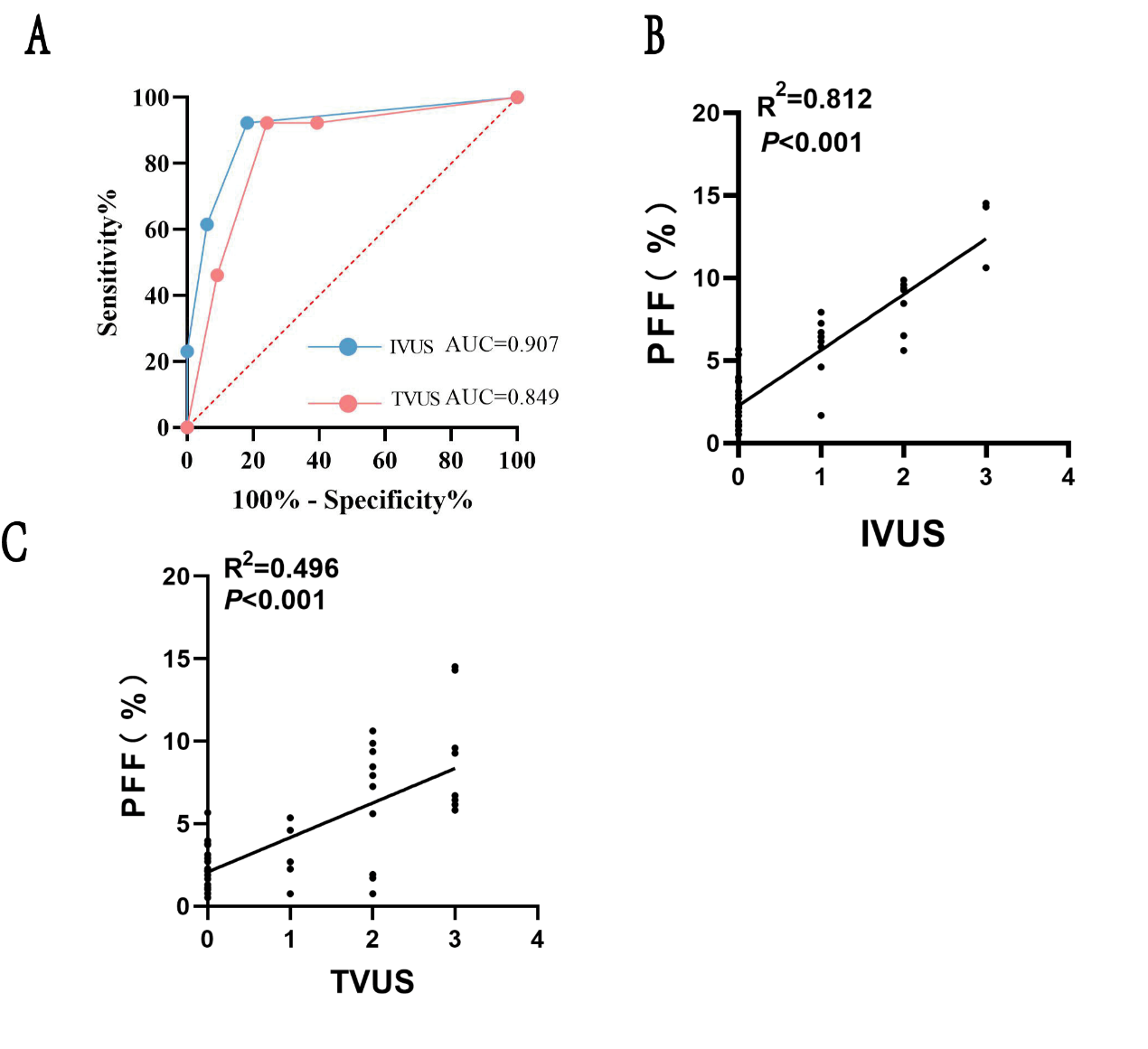
Table 3
Comparison of anthropometric and biochemical parameters of subjects in normal and nonalcoholic fatty pancreatic disease groups and Comparison of visceral fat area and the fat fraction"
| Project | Normal group | NAFPD group | t value | P value |
|---|---|---|---|---|
| Male, cases | 19 (57.6%) | 9 (69.2%) | 0.53 | 0.47 |
| Age, years | 50.77 ± 14.06 | 52.64 ± 12.87 | 0.43 | 0.67 |
| Weight (kg) | 65.67 ± 12.18 | 76.31 ± 12.07 | -2.67 | 0.01 |
| BMI (kg/m2) | 23.93 ± 2.86 | 27.25 ± 2.83 | -3.55 | < 0.01 |
| NAFLD, cases | 12 (38.7%) | 11 (73.3%) | 4.85 | 0.03 |
| TC (mmol/L) | 4.80 ± 0.97 | 4.96 ± 0.41 | -0.52 | 0.61 |
| TG (mmol/L) | 1.42 ± 0.58 | 2.13 ± 1.58 | -2.09 | 0.04 |
| HDL-C (mmol/L) | 1.22 ± 0.28 | 1.10 ± 0.30 | 1.25 | 0.22 |
| LDL-C (mmol/L) | 3.22 ± 0.85 | 3.25 ± 0.57 | -0.09 | 0.99 |
| FPG (mmol/L) | 5.99 ± 1.74 | 6.52 ± 2.37 | -0.78 | 0.43 |
| UA (mmol/L) | 349.50 ± 74.70 | 349.80 ± 93.10 | 0.01 | 0.99 |
| ALT (U/L) | 21.00 (15.00, 36.00) | 27.4 (14.00, 54.50) | -0.80 | 0.42 |
| AST (U/L) | 22.00 (17.00, 32.00) | 26.0 0 (18.50, 30.50) | -0.53 | 0.59 |
| TA (cm2) | 118.80 (95.30, 168.20) | 184.00 (156.40, 26.30) | -3.01 | < 0.01 |
| SA (cm2) | 55.50 (42.80, 78.60) | 61.80 (51.5, 87.60) | -1.45 | 0.15 |
| VA (cm2) | 61.50 (38.90, 91.90) | 117.20 (73.30, 168.90) | -2.89 | < 0.01 |
| VFP (%) | 54.30 ± 12.30 | 62.80 ± 12.90 | -2.08 | 0.04 |
| Subcutaneous fat thickness (cm) | 15.10 (13.3, 20.1) | 17.10 (12.9, 24.9) | -1.14 | 0.25 |
| AC (cm) | 87.15 ± 9.13 | 94.94 ± 5.38 | -2.87 | < 0.01 |
| Pancreatic head fat fraction | 1.86 (1.06, 3.84) | 7.60 (5.91, 11.30) | -4.42 | < 0.01 |
| Pancreatic body fat fraction | 2.63 (0.84, 3.92) | 9.75 (7.39, 13.21) | -5.16 | < 0.01 |
| Pancreatic tail fat fraction | 2.17 (0.95, 3.38) | 10.04 (7.72, 12.44) | -4.89 | < 0.01 |
| PFF | 2.15 (1.12, 3.94) | 9.32 (7.43, 10.43) | -5.23 | < 0.01 |
| HFF | 2.81 (1.78, 5.45) | 8.73 (3.74, 13.50) | -2.54 | 0.01 |
Table 4
Analysis of factors associated with nonalcoholic fatty pancreatic disease"
| Project | r value | P value |
|---|---|---|
| Age | 0.20 | 0.18 |
| Weight | 0.43 | < 0.01 |
| BMI | 0.50 | < 0.01 |
| TC | 0.17 | 0.40 |
| TG | 0.33 | 0.05 |
| HDL-c | -0.07 | 0.69 |
| LDL-c | 0.04 | 0.82 |
| FPG | 0.17 | 0.31 |
| TA | 0.45 | < 0.02 |
| SA | 0.28 | 0.06 |
| VA | 0.45 | < 0.02 |
| VFP | 0.31 | 0.03 |
| AC | 0.48 | < 0.01 |
| HFF | 0.36 | 0.01 |
| [1] | Chen Y, Peng Q, Yang Y, Zheng S, Wang Y, Lu W.The prevalence and increasing trends of overweight, general obesity, and abdominal obesity among chinese adults: A repeated cross-sectional study. BMC Public Health 2019;19:1293. |
| [2] | Lockhart SM, O'Rahilly S.When two pandemics meet: Why is obesity associated with increased COVID-19 mortality? Med (N Y) 2020;1:33-42. |
| [3] | Smits MM, van Geenen EJ. The clinical significance of pancreatic steatosis. Nat Rev Gastroenterol Hepatol 2011;8:169-177. |
| [4] | Ogilvie RF. The islands of langerhans in 19 cases of obesity. J. Pathol 1933;37:473-481 |
| [5] | Dite P, Blaho M, Bojkova M, Jabandziev P, Kunovsky L. Nonalcoholic fatty pancreas disease: Clinical consequences. Dig Dis 2020;38:143-149. |
| [6] | Wagner R, Eckstein SS, Yamazaki H, Gerst F, Machann J, Jaghutriz BA, et al. Metabolic implications of pancreatic fat accumulation. Nature Reviews Endocrinology 2022;18:43-54. |
| [7] | Bi Y, Wang JL, Li ML, Zhou J, Sun XL.The association between pancreas steatosis and metabolic syndrome: A systematic review and meta-analysis. Diabetes Metab Res Rev 2019;35:e3142. |
| [8] | Rahier J, Loozen S, Goebbels RM, Abrahem M. The haemochromatotic human pancreas: A quantitative immunohistochemical and ultrastructural study. Diabetologia 1987;30:5-12. |
| [9] | Rofsky NM, Lee VS, Laub G, Pollack MA, Krinsky GA, Thomasson D, et al. Abdominal MR imaging with a volumetric interpolated breath-hold examination. Radiology 1999;212:876-884. |
| [10] | Zhang Y, Zhou Z, Wang C, Cheng X, Wang L, Duanmu Y, et al. Reliability of measuring the fat content of the lumbar vertebral marrow and paraspinal muscles using MRI mdixon-quant sequence. Diagn Interv Radiol 2018;24:302-307. |
| [11] | Sezgin O, Yaraş S, Özdoğan O. Pancreatic steatosis is associated with both metabolic syndrome and pancreatic stiffness detected by ultrasound elastography. Dig Dis Sci 2022;67:293-304. |
| [12] | Della Corte C, Mosca A, Majo F, Lucidi V, Panera N, Giglioni E, et al. Nonalcoholic fatty pancreas disease and nonalcoholic fatty liver disease: More than ectopic fat. Clin Endocrinol (Oxf) 2015;83:656-662. |
| [13] | Piskin FC, Yavuz S, Kose S, Cagli C, Dogruel D, Tumgor G, et al. A comparative study of the pancreas in pediatric patients with cystic fibrosis and healthy children using two-dimensional shear wave elastography. J Ultrasound 2020;23:535-542. |
| [14] | Smereczyński A, Kołaczyk K.Is a fatty pancreas a banal lesion? Journal of ultrasonography 2016;16:273-280. |
| [15] | Singh RG, Yoon HD, Wu LM, Lu J, Plank LD, Petrov MS. Ectopic fat accumulation in the pancreas and its clinical relevance: A systematic review, meta-analysis, and meta-regression. Metabolism 2017;69:1-13. |
| [16] | Ferraioli G, Monteiro LBS. Ultrasound-based techniques for the diagnosis of liver steatosis. World J Gastroenterol 2019;25:6053-6062. |
| [17] | Johnson ML, Mack LA. Ultrasonic evaluation of the pancreas. Gastrointest Radiol 1978;3:257-266. |
| [18] | Tong X, Dai C, Walker JT, Nair GG, Kennedy A, Carr RM, et al. Lipid droplet accumulation in human pancreatic islets is dependent on both donor age and health. Diabetes 2020;69:342-354. |
| [19] | Rugivarodom M, Geeratragool T, Pausawasdi N, Charatcharoenwitthaya P. Fatty pancreas: Linking pancreas pathophysiology to nonalcoholic fatty liver disease. Journal of clinical and translational hepatology. 2022;10:1229-1239 |
| [20] | Ramkissoon R, Gardner TB. Pancreatic steatosis: An update. Curr Opin Gastroenterol 2019;35:440-447. |
| [21] | Yamazaki H, Tauchi S, Kimachi M, Dohke M, Hanawa N, Kodama Y, et al. Independent association between prediabetes and future pancreatic fat accumulation: A 5-year japanese cohort study. Journal of gastroenterology 2018;53:873-882. |
| [22] | Ramkissoon R, Gardner TB. Pancreatic steatosis: An emerging clinical entity. Am J Gastroenterol 2019;114:1726-1734. |
| [23] | Longo M, Zatterale F, Naderi J, Parrillo L, Formisano P, Raciti GA, et al. Adipose tissue dysfunction as determinant of obesity-associated metabolic complications. Int J Mol Sci 2019;20. |
| [24] | Hansen JB, Dos Santos LRB, Liu Y, Prentice KJ, Teudt F, Tonnesen M, et al. Glucolipotoxic conditions induce β-cell iron import, cytosolic ros formation and apoptosis. J Mol Endocrinol 2018;61:69-77. |
| [25] | Wang X, Misawa R, Zielinski MC, Cowen P, Jo J, Periwal V, et al. Regional differences in islet distribution in the human pancreas--preferential beta-cell loss in the head region in patients with type 2 diabetes PLoS One 2013;8:e67454. |
| [26] | Pfeifer CD, Schoennagel BP, Grosse R, Wang ZJ, Graessner J, Nielsen P, et al. Pancreatic iron and fat assessment by mri-r2* in patients with iron overload diseases. Journal of Magnetic Resonance Imaging 2015;42:196-203. |
| [27] | Gerst F, Wagner R, Oquendo MB, Siegel-Axel D, Fritsche A, Heni M, et al. What role do fat cells play in pancreatic tissue? Mol Metab 2019;25:1-10. |
| [28] | Ranasinghe P, Mathangasinghe Y, Jayawardena R, Hills AP, Misra A.Prevalence and trends of metabolic syndrome among adults in the asia-pacific region: A systematic review. BMC Public Health 2017;17:101. |
| [29] | Ansarimoghaddam A, Adineh HA, Zareban I, Iranpour S, HosseinZadeh A, Kh F. Prevalence of metabolic syndrome in middle-east countries: Meta-analysis of cross-sectional studies. Diabetes Metab Syndr 2018;12:195-201. |
| [30] | Zhou J, Li ML, Zhang DD, Lin HY, Dai XH, Sun XL, et al. The correlation between pancreatic steatosis and metabolic syndrome in a Chinese population. Pancreatology 2016;16:578-583. |
| [1] | Liu Taixia, Wang Hanxiang, Wang Dan, Zhang Yuke, Guo Yunyun, Liu Shuo, Zhang Minfeng, Nie Hongming, Shen Rui. The Role of Sonazoid-contrast-enhanced Ultrasound In Precision Diagnosis and Guidance for Radiofrequency Ablation Therapy of Hepatocellular Carcinoma: a Literature Review [J]. Advanced Ultrasound in Diagnosis and Therapy, 2026, 10(1): 20-28. |
| [2] | Fu Lijia, Li Na, Liao Ziling, Lin Yanping, Li Zhaojun, Li Fan. Advances in Breast Ultrasound Segmentation and Classification [J]. Advanced Ultrasound in Diagnosis and Therapy, 2026, 10(1): 29-41. |
| [3] | Li Na, Li Fan. Focused Ultrasound Combined with Microbubbles for Inducing Blood-Brain Barrier Opening: Cavitation Monitoring and Control [J]. Advanced Ultrasound in Diagnosis and Therapy, 2026, 10(1): 51-58. |
| [4] | Yin Yulian, Cheng Yifan, Zhou Liangmei, Zhong Yuanyuan, Wang Bing, Wu Jingjing, Ren Yajuan, Gao Dongwen, Chen Hongfeng, Ye Meina, Yin Haoqiang. From Non-Mass Stage to Complex Type: Ultrasonographic Assessment of Granulomatous Lobular Mastitis Across Six Clinical Stages [J]. Advanced Ultrasound in Diagnosis and Therapy, 2026, 10(1): 59-68. |
| [5] | Syahril Erlin, Abdullah Nusratuddin, Ilyas Muhammad, As’ad Suryani, Choridah Lina, Natzir Rosdiana, Kurniawan Liong Boy, Bahar Burhanuddin, Mappaware Nasrudin A., Mulyadi Farah Ekawati, Yacca Susdiaman Sudin. The Effects of Ajwa Dates Consumption (Phoenix dactylifera L), on Ovarian Follicular Features with Transvaginal Ultrasound in Perimenopausal Women [J]. Advanced Ultrasound in Diagnosis and Therapy, 2026, 10(1): 69-73. |
| [6] | Si Jiahao, Zhang Ye, Wang Shuaiyanga, Hao Liuwei, Duan Shaobo. Ultrasound-Guided Portal Vein Puncture for The Treatment of Hepatic Portal Venous Gas: A Case Report [J]. Advanced Ultrasound in Diagnosis and Therapy, 2026, 10(1): 74-78. |
| [7] | Guan Xin, Hu Xinyuan, Han Hong, Zhang Dezhi, Xu Huixiong. The Evolving Application of Ultrasound in the Precision Management of Small Hepatocellular Carcinoma [J]. Advanced Ultrasound in Diagnosis and Therapy, 2025, 9(4): 375-387. |
| [8] | Li Yanran, Cui Yuanjie, Wu Qingqing, Zhang Na. Current Applications of Artificial Intelligence in Obstetric Ultrasound [J]. Advanced Ultrasound in Diagnosis and Therapy, 2025, 9(4): 449-456. |
| [9] | Hou Wenfei, Chen Wanting, Liu Huazhen, Tang Jiajia, Yang Meng. Applications of Ultrasound Localization Microscopy in Abdominal Imaging [J]. Advanced Ultrasound in Diagnosis and Therapy, 2025, 9(4): 347-356. |
| [10] | Yu Xiao jie, Song Zheng lai, Chang Xue yong, Yu Jie, Liang Ping. Artificial Intelligence in Ultrasound Diagnosis of Liver Nodules: A Comprehensive Review of B-Mode and Contrast-enhanced Applications [J]. Advanced Ultrasound in Diagnosis and Therapy, 2025, 9(4): 326-346. |
| [11] | Zhong Xian, Xie Xiaoyan. Multimodal Ultrasound Radiomics in Liver Disease: Current Status and Future Directions [J]. Advanced Ultrasound in Diagnosis and Therapy, 2025, 9(4): 388-408. |
| [12] | Zhang Xiaoqian, Zhang Jingwen, Dong Yijie, Zhou Jianqiao. Research Progress and Clinical Translation of Photoacoustic–ultrasound Fusion Imaging in Breast Cancer Diagnosis and Therapy [J]. Advanced Ultrasound in Diagnosis and Therapy, 2025, 9(4): 467-482. |
| [13] | Jin Tong, Yu Xiaohu, Ai Zheng, Guo Hongcheng. Artificial Intelligence in Ultrasound Imaging: A Review of Progress from Machine Learning to Large Language Model [J]. Advanced Ultrasound in Diagnosis and Therapy, 2025, 9(4): 483-496. |
| [14] | Xiang Xi, Yang Yujia, Wang Liyun, Qiu Li. Advances and Applications in Dermatological Ultrasound [J]. Advanced Ultrasound in Diagnosis and Therapy, 2025, 9(4): 457-466. |
| [15] | Zheng Hairong, Meng Long, Li Fei, Niu Lili, Qiu Weibao, Ma Teng, Liu Chengbo, Zhu Xuefeng, Wan Liwen, Cai Feiyan. Advance in Ultrasound Super-resolution Imaging, Cell Manipulation and Inter-brain Communication [J]. Advanced Ultrasound in Diagnosis and Therapy, 2025, 9(4): 307-325. |
| Viewed | ||||||
|
Full text |
|
|||||
|
Abstract |
|
|||||
Share: WeChat
Copyright ©2018 Advanced Ultrasound in Diagnosis and Therapy
|
 Advanced Ultrasound in Diagnosis and Therapy (AUDT)
is licensed under a Creative Commons Attribution 4.0 International License.
Advanced Ultrasound in Diagnosis and Therapy (AUDT)
is licensed under a Creative Commons Attribution 4.0 International License.
