Advanced Ultrasound in Diagnosis and Therapy ›› 2026, Vol. 10 ›› Issue (1): 20-28.doi: 10.26599/AUDT.2026.250084
Previous Articles Next Articles
Liu Taixiaa, Wang Hanxianga, Wang Dana, Zhang Yukea, Guo Yunyuna, Liu Shuoa, Zhang Minfengb, Nie Hongmingc,*( ), Shen Ruia,*(
), Shen Ruia,*( )
)
Received:2025-08-05
Revised:2025-10-19
Accepted:2025-11-21
Online:2026-03-31
Published:2026-03-30
Contact:
Department of Liver Disease, Shanghai Municipal Hospital of Traditional Chinese Medicine, Shanghai University of Traditional Chinese Medicine, Shanghai 200071, China (Hongming Nie), e-mail: beining0630@126.com(HM N);
Department of Ultrasound, Shanghai Municipal Hospital of Traditional Chinese Medicine, Shanghai University of Traditional Chinese Medicine, Shanghai 200071, China (Rui Shen), e-mail: shenrui@shutcm.edu.cn(R S),
Liu Taixia, Wang Hanxiang, Wang Dan, Zhang Yuke, Guo Yunyun, Liu Shuo, Zhang Minfeng, Nie Hongming, Shen Rui. The Role of Sonazoid-contrast-enhanced Ultrasound In Precision Diagnosis and Guidance for Radiofrequency Ablation Therapy of Hepatocellular Carcinoma: a Literature Review. Advanced Ultrasound in Diagnosis and Therapy, 2026, 10(1): 20-28.
Figure 2
Case 1. Sonazoid-enhanced US images were obtained from a 48-year-old male patient diagnosed with chronic viral hepatitis B. B-mode US showed a 16 × 11 mm vaguely defined hypoechoic lesion (A, white arrow), while with Sonazoid-enhanced a part of the lesion showed hyper-enhancement (B, white arrow) and the rest lesion presented hypo-enhancement (C, green area) during the Kupffer phase. Its diagnosis was early HCC (High grade dysplastic nodules with a part of HCC). Finally, the lesion was confirmed to be early-stage HCC by contrast-enhanced MRI."
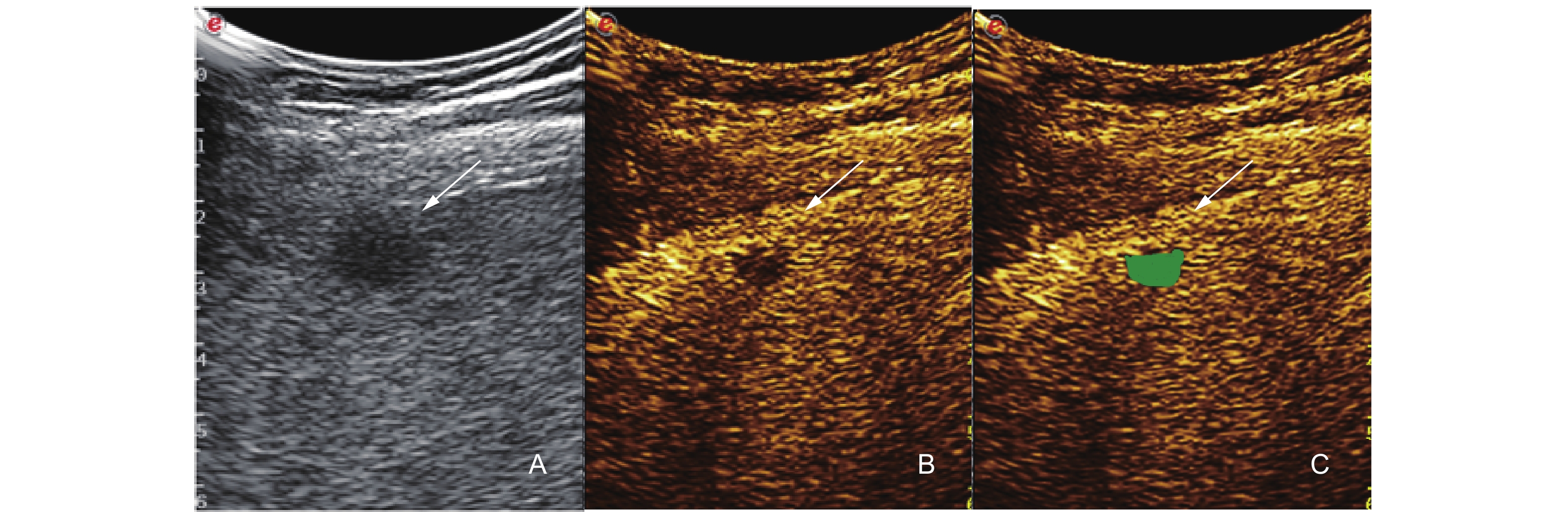
Table 1
Comparison of physical characteristics between Sonazoid-CEUS and SonoVue-CEUS."
| Characteristics | Sonazoid | SonoVue |
| Gas | Perfluorobutane | Sulfur hexafluoride |
| Diameter | 2 um | 2.5 um |
| Shell | Sodium hydrolecithinylserine | Distearoyl hosphatidylcholine |
| Characteristic | Transpulmonary circulation blood vessel + organ specific imaging | Transpulmonary circulation angiography |
Figure 3
Case 2. Sonazoid-enhanced US images were obtained from a 32-year-old male patient diagnosed with chronic viral hepatitis B. The lesion demonstrated nonrim arterial phase hyperenhancement (APHE) (A, white arrow) and early washout (B, white arrow) in the portal venousl phase and manifested an enhancement defect in the subsequent Kupffer phase (C, white arrow). Time-intensity Curve Analysis of HCC using Sonazoid-CEUS (D, yellow line presents HCC after reperfusion Sonazoid-enhanced, red line presents Hepatic parenchyma after reperfusion Sonazoid-enhanced). The lesion confirmed HCC by contrast-enhanced MRI."
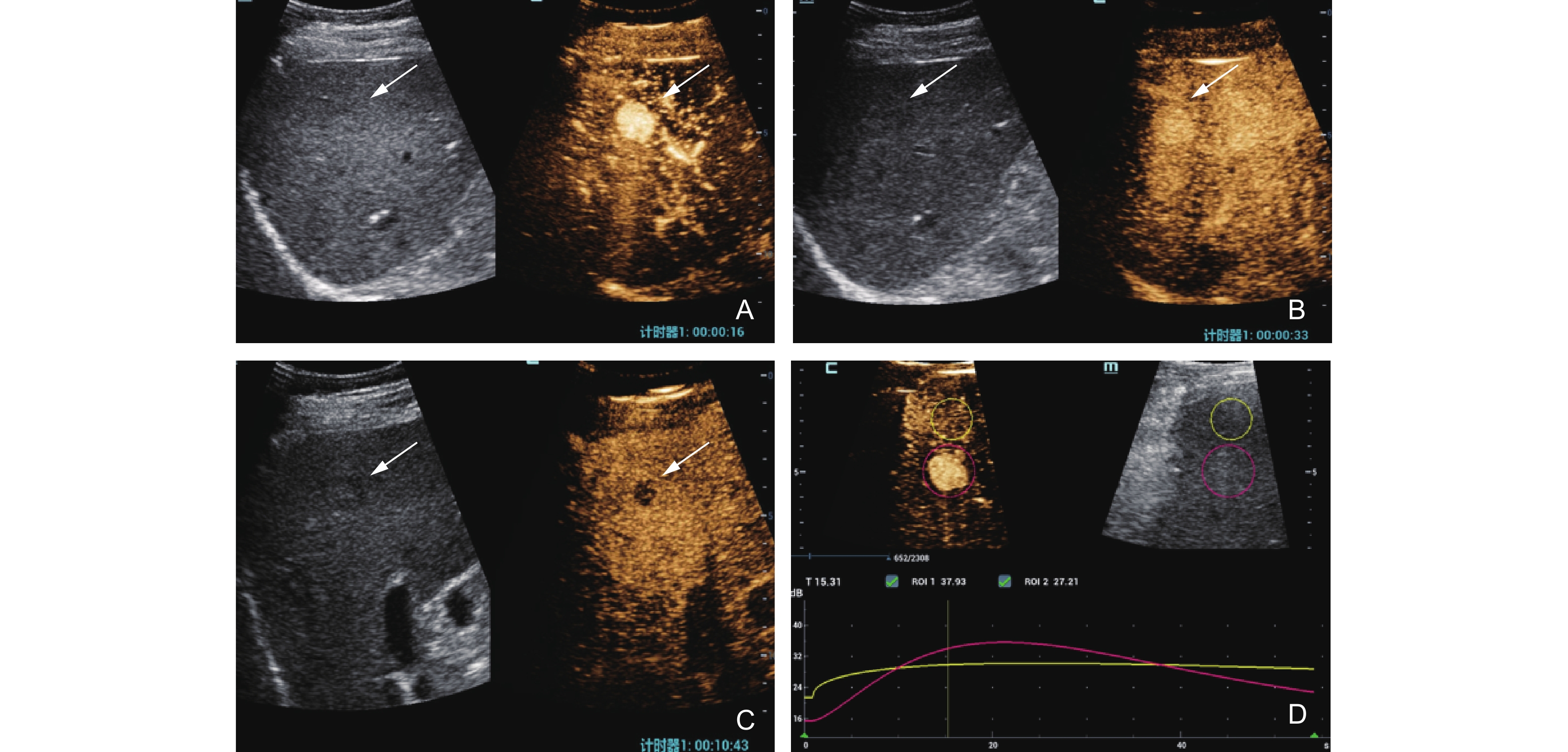
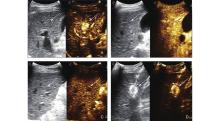
Figure 4
Case 3. Sonazoid-enhanced US images were obtained from a 67-year-old male patient diagnosed with chronic viral hepatitis B. On Sonazoid-enhanced US, the lesion demonstrated to have APHE (A, white arrow) and mild hyperenhancement in one minute (B, white arrow), while manifested hypo-enhancement from 10 minutes in the Kupffer phase (C, white arrow). The lesion was under RFA therapy in the Kupffer phase (D, white arrow). The lesion was ultimately confirmed to be HCC by contrast-enhanced MRI."
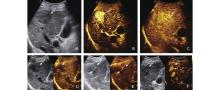
Figure 5
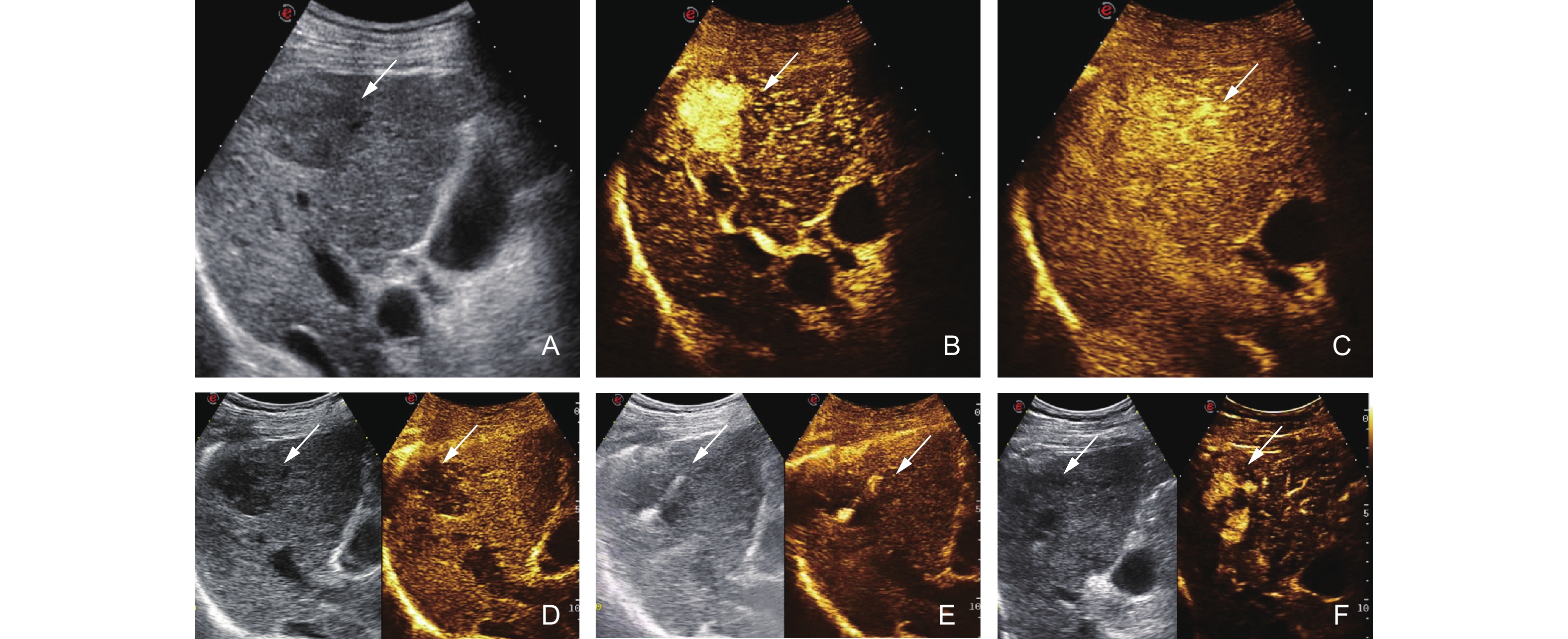
Case 4. Sonazoid-enhanced US images were obtained from a 61-year-old male patient diagnosed with chronic viral hepatitis B. B-mode US image showed a 39mm hypoecho liver lesion (A, white arrow) in hepatic segment VII, the lesion manifested hyper-enhancement during the arterial phase (B, white arrow) and showed subsequent iso-enhancement (26 seconds after contrast agent administration) and was no wash-out in the late phase to 5 minutes on CEUS (C, white arrow), then demonstrated an enhancement defect in the subsequent Kupffer phase (D, white arrow). The lesion was under RFA (E, white arrow). After six months the recurrence besides the lesion could be diagnosed (F, white triangle). The lesion was confirmed to be HCC by contrast-enhanced MRI."
| [1] | Rumgay H, Arnold M, Ferlay J, Lesi O, Cabasag CJ, Vignat J, et al. Global burden of primary liver cancer in 2020 and predictions to 2040. J Hepatol 2022; 77: 1598-1606. |
| [2] | Sung H, Ferlay J, Siegel RL, Laversanne M, Soerjomataram I, Jemal A, et al. Global cancer statistics 2020: GLOBOCAN estimates of incidence and mortality worldwide for 36 cancers in 185 countries. CA Cancer J Clin 2021; 71: 209-249. |
| [3] | Dodd GD, Soulen MC, Kane RA, Livraghi T, Lees WR, Yamashita Y, et al. Minimally invasive treatment of malignant hepatic tumors: at the threshold of a major breakthrough. Radiographics 2000; 20: 9-27. |
| [4] | Taibbi A, Furlan A, Sandonato L, Bova V, Galia M, Marin D, et al. Imaging findings of liver resection using a bipolar radiofrequency electrosurgical device—initial observations. Eur J Radiol 2012; 81: 663-670. |
| [5] |
European Association for the Study of the Liver; European Organisation for Research, Treatment of Cancer. EASL–EORTC clinical practice guidelines: management of hepatocellular carcinoma. J Hepatol 2012; 56: 908-943.
doi: 10.1016/j.jhep.2011.12.001 |
| [6] | Department of Medical Administration, National Health Commission of the People's Republic of China, Clinical practice guideline for primary liver cancer (2024 edition). Med J PUMCH 2024;15:532-559. |
| [7] | Bruix J, Sherman M. Management of hepatocellular carcinoma: an update. Hepatology 2011; 53: 1020-1022. |
| [8] | Livraghi T, Meloni F, Di Stasi M, Rolle E, Solbiati L, Tinelli C, et al. Sustained complete response and complications rates after radiofrequency ablation of very early hepatocellular carcinoma in cirrhosis: is resection still the treatment of choice?. Hepatology 2007; 47: 82-89. |
| [9] | Tiong L, Maddern GJ. Systematic review and meta-analysis of survival and disease recurrence after radiofrequency ablation for hepatocellular carcinoma. Br J Surg 2011; 98: 1210-1224. |
| [10] | Tanaka T, Ikeda K, Sorin Y, Fukushima T, Kawamura Y, Kobayashi M, et al. Three-dimensional imaging using contrast-enhanced and three-dimensional ultrasound techniques in the ablative zone treated with a multipolar radiofrequency ablation system for hepatocellular carcinoma. Oncology 2016; 90: 255-260. |
| [11] | Leen E, Kumar S, Khan SA, Low G, Ong KO, Tait P, et al. Contrast-enhanced 3D ultrasound in the radiofrequency ablation of liver tumors. World J Gastroenterol 2009; 15: 289-299. |
| [12] | Rajesh S, Mukund A, Arora A, Jain D, Sarin SK. Contrast-enhanced US-guided radiofrequency ablation of hepatocellular carcinoma. J Vasc Interv Radiol 2013; 24: 1235-1240. |
| [13] | Pan T, Xie QK, Lv N, Li XS, Mu LW, Wu PH, et al. Percutaneous CT-guided radiofrequency ablation for lymph node oligometastases from hepatocellular carcinoma: a propensity score-matching analysis. Radiology 2017; 282: 259-270. |
| [14] | Inoue T, Kudo M, Hatanaka K, Arizumi T, Takita M, Kitai S, et al. Usefulness of contrast-enhanced ultrasonography to evaluate the post-treatment responses of radiofrequency ablation for hepatocellular carcinoma: comparison with dynamic CT. Oncology 2013; 84: 51-57. |
| [15] | Marrero JA, Kulik LM, Sirlin CB, Zhu AX, Finn RS, Abecassis MM, et al. Diagnosis, staging, and management of hepatocellular carcinoma: 2018 practice guidance by the American Association for the Study of Liver Diseases. Hepatology 2018; 68: 723-750. |
| [16] | Dietrich CF, Nolsøe CP, Barr RG, Berzigotti A, Burns PN, Cantisani V, et al. Guidelines and good clinical practice recommendations for contrast-enhanced ultrasound (CEUS) in the liver-update 2020 WFUMB in cooperation with EFSUMB, AFSUMB, AIUM, and FLAUS. Ultrasound Med Biol 2020; 46: 2579-2604. |
| [17] | Claudon M, Dietrich CF, Choi BI, Cosgrove DO, Kudo M, Nolsøe CP, et al. Guidelines and good clinical practice recommendations for contrast enhanced ultrasound (CEUS) in the liver--update 2012: a WFUMB-EFSUMB initiative in cooperation with representatives of AFSUMB, AIUM, ASUM, FLAUS and ICUS. Ultraschall Med 2013; 34: 11-29. |
| [18] | Bansa S, Gui J, Merrill C, Wong JK, Burak KW, Wilson SR. Contrast-enhanced US in local ablative therapy and secondary surveillance for hepatocellular carcinoma. RadioGraphics 2019; 39: 1302-1322. |
| [19] | Numata K, Luo W, Morimoto M, Kondo M, Kunishi Y, Sasaki T, et al. Contrast enhanced ultrasound of hepatocellular carcinoma. World J Radiol 2010; 2: 68-82. |
| [20] | Yanagisawa K, Moriyasu F, Miyahara T, Yuki M, Iijima H. Phagocytosis of ultrasound contrast agent microbubbles by Kupffer cells. Ultrasound Med Biol 2007; 33: 318-325. |
| [21] | Lee J, Minami Y, Choi B, Lee W, Chou YH, Jeong W, et al. The AFSUMB consensus statements and recommendations for the clinical practice of contrast-enhanced ultrasound using Sonazoid. J Med Ultrasound 2020; 28: 59-82. |
| [22] | Kudo M, Hatanaka K, Kumada T, Toyoda H, Tada T. Double-contrast ultrasound: a novel surveillance tool for hepatocellular carcinoma. Am J Gastroenterol 2011; 106: 368-370. |
| [23] | Kudo M, Ueshima K, Osaki Y, Hirooka M, Imai Y, Aso K, et al. B-mode ultrasonography versus contrast-enhanced ultrasonography for surveillance of hepatocellular carcinoma: a prospective multicenter randomized controlled trial. Liver Cancer 2019; 8: 271-280. |
| [24] | Goto E, Masuzaki R, Tateishi R, Kondo Y, Imamura J, Goto T, et al. Value of post-vascular phase (Kupffer imaging) by contrast-enhanced ultrasonography using Sonazoid in the detection of hepatocellular carcinoma. J Gastroenterol 2012; 47: 477-485. |
| [25] | Park JH, Park MS, Lee SJ, Jeong WK, Lee JY, Park MJ, et al. Contrast-enhanced US with perfluorobutane (Sonazoid) used as a surveillance test for hepatocellular carcinoma (HCC) in Cirrhosis (SCAN): an exploratory cross-sectional study for a diagnostic trial. BMC Cancer 2017; 17: 279. |
| [26] | Ohama H, Imai Y, Nakashima O, Kogita S, Takamura M, Hori M, et al. Images of Sonazoid-enhanced ultrasonography in multistep hepatocarcinogenesis: comparison with Gd-EOB-DTPA-enhanced MRI. J Gastroenterol 2014; 49: 1081-1093. |
| [27] | Ding J, Zhou Y, Wang Y, Zhou H, Jing X. Clinical value of contrast-enhanced ultrasound in differential diagnosis of early hepatocellular carcinoma and dysplastic nodules. AUDT 2017; 01: 010-014. |
| [28] | Hwang JA, Jeong WK, Kang HJ, Lee ES, Park HJ, Lee JM. Perfluorobutane-enhanced ultrasonography with a Kupffer phase: improved diagnostic sensitivity for hepatocellular carcinoma. Eur Radiol 2022; 32: 8507-8517. |
| [29] | Bokor D, Chambers JB, Rees PJ, Mant TG, Luzzani F, Spinazzi A. Clinical safety of SonoVue, a new constrast agent for ultrasound imaging, in healthy volunteers and in patients with chronic obstructive pulmonary disease. Invest Radiol 2001; 36: 104-109. |
| [30] | Landmark KE, Johansen PW, Johnson JA, Johansen B, Uran S, Skotland T. Pharmacokinetics of perfluorobutane following instravenous bolus injection and continuous infusion of sonazoid in healthy volunteers and in patients with reduced pulmonary diffusing capacity. Ultrasoubd Med Biol 2008; 34: 494-501. |
| [31] | Hvattum E, Uran S, Sandbaek AG, Karlsson AA, Skotland T. Quantification of phosphatidy lserine, phosphatidic acid and free fatty acids in an ultrasound contrast agent by normal-phase high-performance liquid chromatography with evaporative light scattering detection. J Pharm Biomed Anal 2006; 42: 506-512. |
| [32] | Kang HJ, Lee JM, Yoon JH, Yoo J, Choi Y, Joo I, et al. SonazoidTM versus SonoVue® for diagnosing hepatocellular carcinoma using contrast-enhanced ultrasound in at-risk individuals: a prospective, single-center, intraindividual, noninferiority study. Korean J Radiol 2022; 23: 1067-1077. |
| [33] | Kang HJ, Lee JM, Yoon JH, Lee K, Kim H, Han JK. Contrast-enhanced US with sulfur hexafluoride and perfluorobutane for the diagnosis of hepatocellular carcinoma in individuals with high risk. Radiology 2020; 297: 108-116. |
| [34] | Huang J, Gao L, Li J, Yang R, Jiang Z, Liao M, et al. Head-to-head comparison of Sonazoid and SonoVue in the diagnosis of hepatocellular carcinoma for patients at high risk. Front Oncol 2023; 13: 1140277. |
| [35] | Zhai H, Liang P, Yu J, Cao F, Kuang M, Liu F, et al. Comparison of Sonazoid and SonoVue in the diagnosis of focal liver lesions: a preliminary study. J Ultrasound Med 2019; 38: 2417-2425. |
| [36] | Hatanaka K, Kudo M, Minami Y, Maekawa K. Sonazoid-enhanced ultrasonography for diagnosis of hepatic malignancies: comparison with contrast-enhanced CT. Oncology 2008; 75: 42-47. |
| [37] | Yang WY, Park HS, Kim YJ, Yu MH, Jung SI, Jeon HJ. Visibility of focal liver lesions: comparison between Kupffer phase of CEUS with Sonazoid and hepatobiliary phase of gadoxetic acid-enhanced MRI. J Clin Ultrasound 2017; 45: 542-550. |
| [38] | Imai Y, Murakami T, Yoshida S, Nishikawa M, Ohsawa M, Tokunaga K, et al. Superparamagnetic iron oxide-enhanced magnetic resonance images of hepatocellular carcinoma: correlation with histological grading. Hepatology 2000; 32: 205-212. |
| [39] | Inoue T, Kudo M, Hatanaka K, Takahashi S, Kitai S, Ueda T, et al. Imaging of hepatocellular carcinoma: qualitative and quantitative analysis of postvascular phase contrast-enhanced ultrasonography with Sonazoid. Oncology 2008; 75: 48-54. |
| [40] | Korenaga K, Korenaga M, Furukawa M, Yamasaki T, Sakaida I. Usefulness of Sonazoid contrast-enhanced ultrasonography for hepatocellular carcinoma: comparison with pathological diagnosis and superparamagnetic iron oxide magnetic resonance images. J Gastroenterol 2009; 44: 733-741. |
| [41] | Numata K, Morimoto M, Ogura T, Sugimori K, Takebayashi S, Okada M, et al. Ablation therapy guided by contrast-enhanced sonography with Sonazoid for hepatocellular carcinoma lesions not detected by conventional sonography. J Ultrasound Med 2008; 27: 395-406. |
| [42] | Bouwens L, Baekeland M, De Zanger R, Wisse E. Quantitation, tissue distribution and proliferation kinetics of Kupffer cells in normal rat liver. Hepatology 1986; 6: 718-722. |
| [43] | Tanaka M, Nakashima O, Wada Y, Kage M, Kojiro M. Pathomorphological study of Kupffer cells in hepatocellular carcinoma and hyperplastic nodular lesions in the liver. Hepatology 1996; 24: 807-812. |
| [44] | Kang HJ, Kim JH, Yoo J, Han JK. Diagnostic criteria of perfluorobutane-enhanced ultrasonography for diagnosing hepatocellular carcinoma in high-risk individuals: how is late washout determined?. Ultrasonography 2022; 41: 530-542. |
| [45] | Sugimoto K, Moriyasu F, Saito K, Taira J, Saguchi T, Yoshimura N, et al. Comparison of kupffer-phase Sonazoid-enhanced sonography and hepatobiliary-phase gadoxetic acid-enhanced magnetic resonance imaging of hepatocellular carcinoma and correlation with histologic grading. J Ultrasound Med 2012; 31: 529-538. |
| [46] | Zou RH, Lin QG, Huang W, Li XL, Cao Y, Zhang J, et al. Quantitative contrast-enhanced ultrasonic imaging reflects microvascularization in hepatocellular carcinoma and prognosis after resection. Ultrasound Med Biol 2015; 41: 2621-2630. |
| [47] | Gatos I, Tsantis S, Spiliopoulos S, Skouroliakou A, Theotokas I, Zoumpoulis P, et al. A New Automated Quantification Algorithm for the Detection and Evaluation of Focal Liver Lesions with Contrast‐enhanced Ultrasound. Medical Physics 2015; 42: 3948-3959. |
| [48] | Kondo S, Takagi K, Nishida M, Iwai T, Kudo Y, Ogawa K, et al. Computer-aided diagnosis of focal liver lesions using contrast-enhanced ultrasonography with perflubutane microbubbles. IEEE Trans Med Imaging 2017; 36: 1427-1437. |
| [49] | Guo LH, Wang D, Qian YY, Zheng X, Zhao CK, Li XL, et al. A two-stage multi-view learning framework based computer-aided diagnosis of liver tumors with contrast enhanced ultrasound images. Clin Hemorheol Microcirc 2018; 69: 343-354. |
| [50] | Wang Z, Yao J, Jing X, Li K, Lu S, Yang H, et al. A combined model based on radiomics features of sonazoid contrast-enhanced ultrasound in the kupffer phase for the diagnosis of well-differentiated hepatocellular carcinoma and atypical focal liver lesions: a prospective, multicenter study. Abdom Radiol 2024; 49: 3427-3437. |
| [51] | Zuo D, Cao JY, Qiu YY, Wang HZ, Tian XF, Wang WP, et al. Radiomics study on predictive model of microvascular invasion in hepatocellular carcinoma based on kupffer phase image of Sonazoid contrast-enhanced ultrasound. J Clin Ultrasound 2022; 24: 485-489. |
| [52] | Zhang Y, Wei Q, Huang Y, Yao Z, Yan C, Zou X, et al. Deep learning of liver contrast-enhanced ultrasound to predict microvascular invasion and prognosis in hepatocellular carcinoma. Front Oncol 2022; 12: 878061. |
| [53] | Qin Q, Wen R, Bai XM, Gao RZ, Yang YP, Gan XY, et al. Deep learning based on kupffer phase of Sonazoid contrast-enhanced ultrasound to predict microvascular invasion in hepatocellular carcinoma. Oncoradiology 2024; 33: 432-441. |
| [54] | Sugimoto K, Kakegawa T, Takahashi H, Tomita Y, Abe M, Yoshimasu Y, et al. Usefulness of modified CEUS LI-RADS for the diagnosis of hepatocellular carcinoma using Sonazoid. Diagnostics 2020; 10: 828. |
| [55] | Sugimoto K, Saito K, Shirota N, Kamiyama N, Sakamaki K, Takahashi H, et al. Comparison of modified CEUS LI-RADS with Sonazoid and CT/MRI LI-RADS for diagnosis of hepatocellular carcinoma. Hepatol Res 2022; 52: 730-738. |
| [56] | Hwang JA, Jeong WK, Min JH, Kim YY, Heo NH, Lim HK. Sonazoid-enhanced ultrasonography: comparison with CT/MRI Liver Imaging Reporting and Data System in patients with suspected hepatocellular carcinoma. Ultrasonography 2021; 40: 486-498. |
| [57] | Liao W, Que Q, Wen R, Lin P, Chen Y, Pang J, et al. Comparison of the feasibility and diagnostic performance of ACR CEUS LI‐RADS and a modified CEUS LI‐RADS for HCC in examinations using Sonazoid. J Ultrasound Med 2023; 42: 2501-2511. |
| [58] | Pox C, Aretz S, Bischoff S, Graeven U, Hass M, Heußner P, et al. S3-Leitlinie Kolorektales KarzinomVersion 1.0-Juni 2013 AWMF-Registernummer: 021/007OL. Z Gastroenterol 2013; 51: 753-854. |
| [59] | Minami Y, Kudo M. Imaging modalities for assessment of treatment response to nonsurgical hepatocellular carcinoma therapy: contrast-enhanced US, CT, and MRI. Liver Cancer 2015; 4: 106-114. |
| [60] | Gao Y, Zheng DY, Cui Z, Ma Y, Liu YZ, Zhang W. Predictive value of quantitative contrast-enhanced ultrasound in hepatocellular carcinoma recurrence after ablation. World J Gastroenterol 2015; 21: 10418-10426. |
| [61] | Park HS, Kim YJ, Yu MH, Jung SI, Jeon HJ. Real‐time contrast‐enhanced sonographically guided biopsy or radiofrequency ablation of focal liver lesions using perflurobutane microbubbles (Sonazoid): value of kupffer‐phase imaging. J Ultrasound Med 2015; 34: 411-421. |
| [62] | Moriyasu F, Itoh K. Efficacy of perflubutane microbubble-enhanced ultrasound in the characterization and detection of focal liver lesions: phase 3 multicenter clinical trial. AJR Am J Roentgenol 2009; 193: 86-95. |
| [63] | Kudo M. Defect reperfusion imaging with Sonazoid®: a breakthrough in hepatocellular carcinoma. Liver Cancer 2016; 5: 1-7. |
| [64] | Kim TK, Jang HJ. Contrast-enhanced ultrasound in the diagnosis of nodules in liver cirrhosis. World J Gastroenterol 2014; 20: 3590-3596. |
| [65] | Martin RC 2nd, Reuter NP, Woodall C. Intra-operative contrast-enhanced ultrasound improves image enhancement in the evaluation of liver tumors. J Surg Oncol 2010; 101: 370-375. |
| [66] | Nishigaki Y, Hayashi H, Tomita E, Suzuki Y, Watanabe N, Watanabe S, et al. Usefulness of Contrast‐enhanced ultrasonography using Sonazoid for the assessment of therapeutic response to percutaneous radiofrequency ablation for hepatocellular carcinoma. Hepatol Res 2015; 45: 432-440. |
| [1] | Xu Junmei, Tahmasebi Aylin, Mohammed Amr, Pour Bahareh Kian, Liu Ji-Bin, Eisenbrey John R.. Contrast-enhanced Ultrasound LI-RADS for Nonradiation Treatment Response Assessment in Liver Tumor: A Pictorial Review Based on LR-TR v2024 [J]. Advanced Ultrasound in Diagnosis and Therapy, 2025, 9(4): 357-374. |
| [2] | Yu Xiao jie, Song Zheng lai, Chang Xue yong, Yu Jie, Liang Ping. Artificial Intelligence in Ultrasound Diagnosis of Liver Nodules: A Comprehensive Review of B-Mode and Contrast-enhanced Applications [J]. Advanced Ultrasound in Diagnosis and Therapy, 2025, 9(4): 326-346. |
| [3] | Guan Xin, Hu Xinyuan, Han Hong, Zhang Dezhi, Xu Huixiong. The Evolving Application of Ultrasound in the Precision Management of Small Hepatocellular Carcinoma [J]. Advanced Ultrasound in Diagnosis and Therapy, 2025, 9(4): 375-387. |
| [4] | Yue Tian, MB, Yanan Zhao, MD, Yiran Huang, MB. The Diagnostic Value of Real-time Shear Wave Ultrasound Elastography in the Differentiation of Hepatic Hemangioma and Hepatocellular Carcinoma [J]. Advanced Ultrasound in Diagnosis and Therapy, 2024, 8(3): 124-129. |
| [5] | Osama Mahmoud, BS, Ajay Makkena, BS, Corinne E. Wessner, MS, MBA, RDMS, Ji-Bin Liu, MD, John R. Eisenbrey, PhD, Andrej Lyshchik, MD, PhD. Contrast-Enhanced Ultrasound LI-RADS: A Pictorial Review [J]. Advanced Ultrasound in Diagnosis and Therapy, 2023, 7(4): 321-332. |
| [6] | Esika Savsani, Mohamed Tantawi, MD, Corinne E. Wessner, MBA, RDMS, RVT, Philip Lee, MD, Andrej Lyshchik, MD, PhD, Kevin Anton, MD, PhD, Colette M. Shaw, MD, Ji-Bin Liu, MD, John R. Eisenbrey, PhD. Contrast-enhanced Ultrasound Assessment of Treatment Response in a Patient with Multifocal Hepatocellular Carcinoma Treated with Transarterial Chemo and Radioembolization [J]. Advanced Ultrasound in Diagnosis and Therapy, 2021, 5(3): 254-257. |
| [7] | Mengna He, MD, PHD, Lu Zhu, MD, Tianan Jiang, MD, PHD. Findings of Fat Containing Hepatocellular Carcinoma on Contrast-enhanced Ultrasound with Sonazoid: A Case Report [J]. Advanced Ultrasound in Diagnosis and Therapy, 2021, 5(2): 98-101. |
| [8] | Yan Zhou, Jianmin Ding, Fengmei Wang, Zhengyi Qin, Yandong Wang, Hongyu Zhou, Xiang Jing. The Effects of Liver Function Damage after Thermal Ablation on the Prognosis of HCC Patients and Its Prediction [J]. Advanced Ultrasound in Diagnosis and Therapy, 2021, 5(2): 80-86. |
| [9] | Danni He, MS, Qiao Ji, MD, Huitong Lin, MD, Xuankun Liang, MM, Lujing Li, MM, Fengping Liang, MM, Xianxiang Wang, MM, Kun Yuan, MS, Zuofeng Xu, MD. A New-Designed Microwave Ablation System: Testing in ex vivo and in vivo Liver Model [J]. Advanced Ultrasound in Diagnosis and Therapy, 2021, 5(1): 39-46. |
| [10] | Tong Zhang, MD, Wenzhao Liang, MD, Yuanyuan Song, MD, Zhengmin Wang, MD, Dezhi Zhang, MD. US-CT Fusion Image-Guided Microwave Ablation of Lung Cancer----A New Mode of Image Guidance in Lung Cancer Ablation [J]. Advanced Ultrasound in Diagnosis and Therapy, 2020, 4(4): 343-348. |
| [11] | Ruiqing Liu, MD, Yaqiong Li, PhD, Bing Mao, MD, Na Li, PhD, Shaobo Duan, MD, Zhiyang Chang, MS, Ye Zhang, MS, Shuaiyang Wang, MS, Lianzhong Zhang, MD. Focal Ablation Therapy for Prostate Cancer: A Literature Review [J]. Advanced Ultrasound in Diagnosis and Therapy, 2020, 4(4): 308-314. |
| [12] | Mengna He, MD, PhD, Lei Xu, MD, Tian’an Jiang, MD, PhD. Time-intensity Curve Analysis of Hepatocellular Carcinoma using Two Contrast-enhanced Ultrasound Methods: Contrast Pulse Sequencing and Contrast Harmonic Imaging [J]. Advanced Ultrasound in Diagnosis and Therapy, 2020, 4(3): 217-222. |
| [13] | Li Ma, MD, Wenzhao Liang, MD, Yupeng Zhu, MD, Yingqiao Zhu, MD, Dezhi Zhang, MD. Differences in CEUS and CE-MRI Appearance of HCC: A Case Report [J]. Advanced Ultrasound in Diagnosis and Therapy, 2019, 3(4): 197-199. |
| [14] | Meng Li, MD, Zhiyan Li, MD, Yuejuan Gao, MD, Jiangke Tian, MD, Min Chen, MD, Jinghui Dong, MD. Safety and Efficacy of Percutaneous Radiofrequency Ablation Combined with Percutaneous Ethanol Injection for Hepatocellular Carcinoma in High-risk Locations [J]. Advanced Ultrasound in Diagnosis and Therapy, 2018, 2(1): 1-7. |
| [15] | Xianghong Luo, MD, Qian Zhang, MD, Qing Yan, MD, Jufang Wang, MD, Qingqing Dong, MD, Zhaojun Li, MD. Diagnosis with Echocardiography for Rare Cases of Anomalous Left Main Coronary Artery: Two Case Reports and Important Lessons Learned [J]. Advanced Ultrasound in Diagnosis and Therapy, 2017, 1(1): 15-18. |
| Viewed | ||||||
|
Full text |
|
|||||
|
Abstract |
|
|||||
Share: WeChat
Copyright ©2018 Advanced Ultrasound in Diagnosis and Therapy
|
 Advanced Ultrasound in Diagnosis and Therapy (AUDT)
is licensed under a Creative Commons Attribution 4.0 International License.
Advanced Ultrasound in Diagnosis and Therapy (AUDT)
is licensed under a Creative Commons Attribution 4.0 International License.
