Advanced Ultrasound in Diagnosis and Therapy ›› 2026, Vol. 10 ›› Issue (1): 59-68.doi: 10.26599/AUDT.2026.250053
Previous Articles Next Articles
Yin Yuliana,1, Cheng Yifana,1, Zhou Liangmeib, Zhong Yuanyuana, Wang Binga, Wu Jingjinga, Ren Yajuanb, Gao Dongwenb, Chen Hongfenga, Ye Meinaa,*( ), Yin Haoqiangb,*(
), Yin Haoqiangb,*( )
)
Received:2025-07-16
Revised:2025-10-20
Accepted:2025-11-27
Online:2026-03-31
Published:2026-03-30
Contact:
Department of Traditional Chinese Medicine Breast Surgery, Longhua Hospital, Shanghai University of Traditional Chinese Medicine, Shanghai,China (Meina Ye), e-mail: yemeina2002@126.com(MN Y);
Department of Ultrasound Medicine, Longhua Hospital affiliated to Shanghai University of Traditional Chinese Medicine, Shanghai, China (Haoqiang Yin), e-mail: rvsvpjt20@outlook.com (HQ Y),
About author:1Yulian Yin and Yifan Cheng contributed equally to this study.
Yin Yulian, Cheng Yifan, Zhou Liangmei, Zhong Yuanyuan, Wang Bing, Wu Jingjing, Ren Yajuan, Gao Dongwen, Chen Hongfeng, Ye Meina, Yin Haoqiang. From Non-Mass Stage to Complex Type: Ultrasonographic Assessment of Granulomatous Lobular Mastitis Across Six Clinical Stages. Advanced Ultrasound in Diagnosis and Therapy, 2026, 10(1): 59-68.
Table 2
Distribution of ultrasonographic features in different stages of GLM"
| Ultrasonographic features | Non-mass stage (n = 42) | Mass stage (n = 61) | Abscess stage (n = 33) | Late ulceration stage (n = 27) | Fistula stage (n = 41) | Complex type# (n = 57) | χ2 | P value |
| # Statistical analysis was not included for the Complex Type as this group may exhibit characteristics from the preceding stages, leading to potential confounding and dilution of effects. * Different types of track signs may occur concurrently within the same case; therefore, the sum of the frequencies of each track sign subtype exceeds the total frequency of the track sign (All Types). a Fisher’s exact test; b The imaging features marked in this study are strictly stage-dependent (appearing only in specific pathological stages or later stages), and theoretically, they cannot appear prior to the specified stages (with observed values being 0 in this study). Given their 100% specificity (no false positives observed), we conducted the analysis only on subgroups where these features were actually present. | ||||||||
| Track Ssign * (All types) | 39 (92.86%) | 15 (24.59%) | 4 (12.12%) | 5 (18.52%) | 3 (7.32%) | 31 (54.39%) | 92.207 | < 0.001 |
| Track sign with high echogenicity on the inner wall* | 24 (57.14%) | 7 (11.48%) | 2 (6.06%) | 3 (11.11%) | 2 (4.88%) | 16 (28.07%) | 52.721 | < 0.001 |
| Track sign with low echogenicity on the inner wall* | 17 (40.48%) | 4 (6.56%) | 1 (3.03%) | 1 (3.7%) | 1 (2.44%) | 7 (12.28%) | 31.689a | < 0.001a |
| Track sign with isoechogenicity on the inner wall* | 11 (26.19%) | 2 (3.28%) | 1 (3.03%) | 1 (3.7%) | 1 (2.44%) | 5 (8.77%) | 17.256a | < 0.001a |
| Track sign with periductal abscess formation* | 7 (16.67%) | 2 (3.28%) | 1 (3.03%) | 1 (3.7%) | 1 (2.44%) | 3 (5.26%) | 7.870a | 0.057a |
| Track sign coexisting with ductal inflammation, periductal inflammation, and nodular structures* | 10 (23.81%) | 1 (1.64%) | 1 (3.03%) | 1 (3.7%) | 1 (2.44%) | 6 (10.53%) | 16.773a | <0.001a |
| Donut sign | 29 (69.05%) | 4 (6.56%) | 22 (66.67%) | 2 (7.41%) | 2 (4.88%) | 7 (12.28%) | 88.196 | < 0.001 |
| False burr sign | 0 (0%) | 48 (78.69%) | 2 (6.06%) | 8 (29.63%) | 7 (17.07%) | 17 (29.82%) | 64.005b | < 0.001b |
| Large areas of mixed echogenicity with irregularly thickened and rough abscess walls; a flowing sensation within the abscess cavity was observed upon probe compression. | 0 (0%) | 0 (0%) | 33 (100%) | 8 (29.63%) | 4 (9.76%) | 11 (19.30%) | 63.599b | <0.001b |
| A relatively well-defined and smooth-edged hypoechoic area was observed in the areolar region, communicating with the ductal system. | 0 (0%) | 0 (0%) | 0 (0%) | 19 (70.37%) | 19 (46.34%) | 23 (40.35%) | 3.813b | 0.043b |
| A duct-like hypoechoic structure extending toward the skin was observed, with thickening of the inner wall of the duct. | 0 (0%) | 0 (0%) | 0 (0%) | 3 (7.32%) | 38 (92.68%) | 26 (45.61%) | 21.815b | < 0.001b |

Figure 1
Ultrasonographic features of the Non-Mass Stage in GLM (type 1: Track Sign with High Echogenicity on the Inner Wall). (A) shows the appearance of several ducts behind the areola, exhibiting irregular dilation and thickening of the ductal walls; (B) magnified image, reveals the thickened ductal walls with a strip-like or linear high echogenicity on the inner wall. The duct wall is smooth, and lipid-containing secretions (bold arrow) are visible inside the duct. A thin, uniformly hypoechoic halo (thin arrow) surrounds the duct; (C) highlights the blue region, which represents the hypoechoic track sign due to the thickening around the duct."
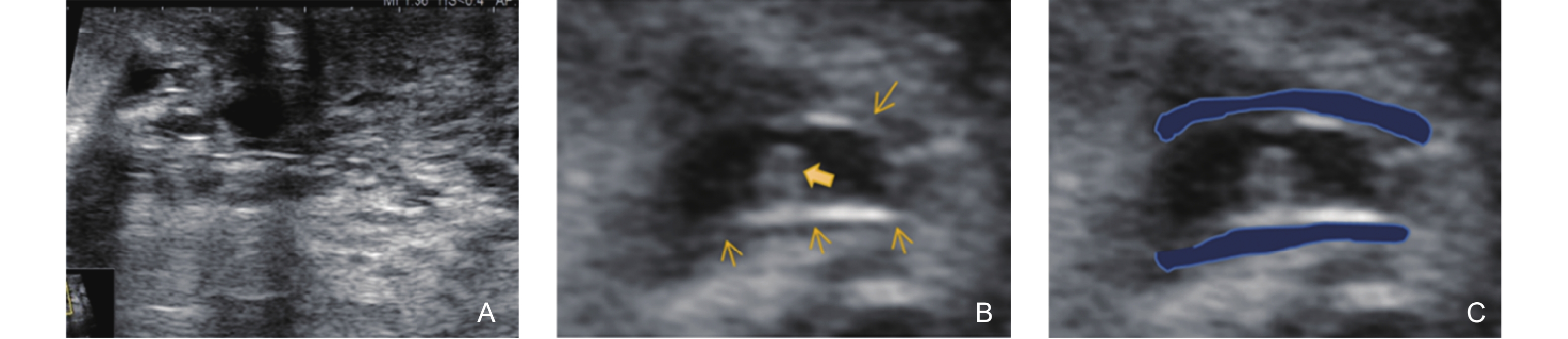

Figure 2
Ultrasonographic features of the Non-Mass Stage in GLM (type 2: Track Sign with Low Echogenicity on the Inner Wall). (A) shows the appearance of several ducts behind the areola with irregular dilation and thickening of the ductal walls; (B) a magnified image, reveals the thickened ductal walls with roughened inner walls. Dense lipid-containing secretions (bold arrow) are visible within the lumen, and a floating sign is observed upon probe compression. A thick, uneven hypoechoic area (thin arrow) surrounds the duct; (C) highlights the blue region, representing the hypoechoic track sign with uneven thickening around the duct."
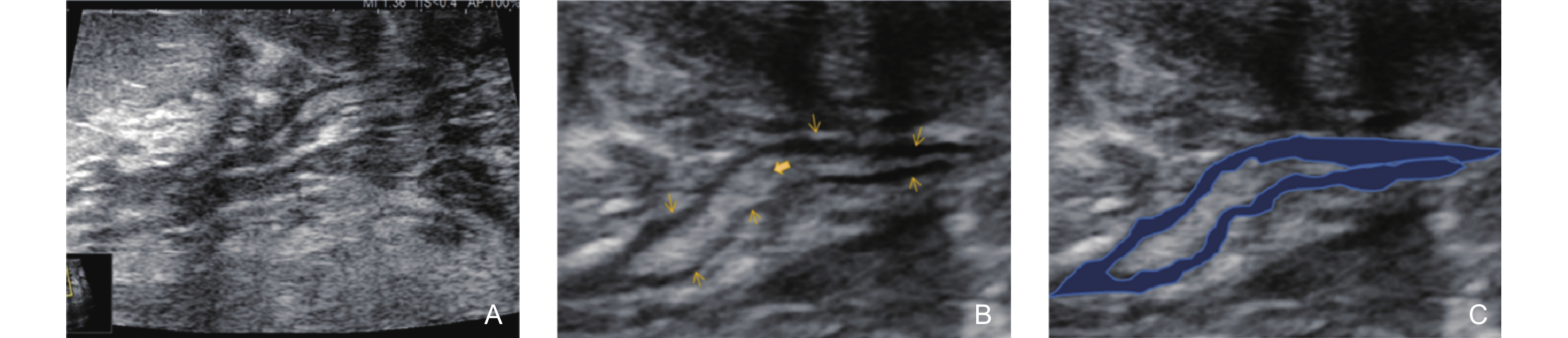
Figure 3
Ultrasonographic features of the Non-Mass Stage in GLM (type 3: Track Sign with isoechogenicity on the Inner Wall). (A) shows the ultrasonographic appearance of several ducts behind the areola with irregular dilation and thickening of the ductal walls; (B) a magnified image, reveals significant thickening of the walls of some ducts, with the inner walls becoming thickened and rough, presenting as isoechoic (triangle arrow). No anechoic secretion is observed within the lumen (bold arrow). The surrounding ductal wall is notably thickened, presenting as an uneven hypoechoic area (thin arrow)."
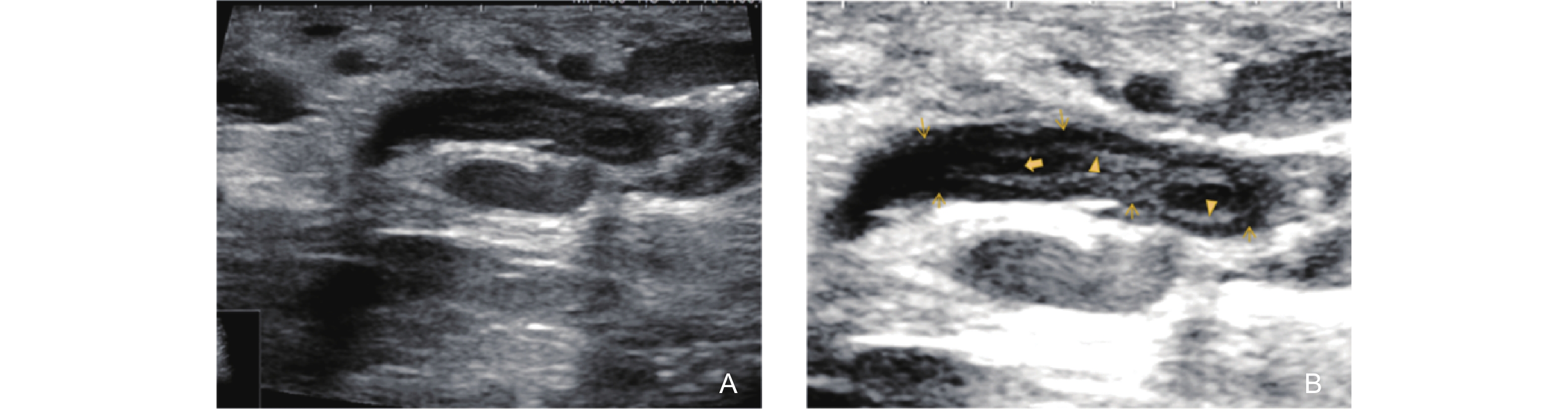
Figure 4
Ultrasonographic features of the Non-Mass Stage in GLM (type 4: Track Sign with Periductal Abscess Formation). (A) shows the ultrasonographic appearance of several ducts behind the areola with irregular dilation. The inner wall of the duct displays linear high echogenicity (triangle arrow), while the surrounding ductal wall is markedly thickened and presents as an extremely hypoechoic area (thin arrow). The stroma around the duct shows decreased echogenicity, slightly higher than that of the surrounding ductal wall (area marked with asterisks); (B) shows the same patient's ipsilateral breast, with a local quadrant demonstrating an irregular mixed echogenic area around the duct, which corresponds to fat necrosis and abscess formation (bold arrow)."
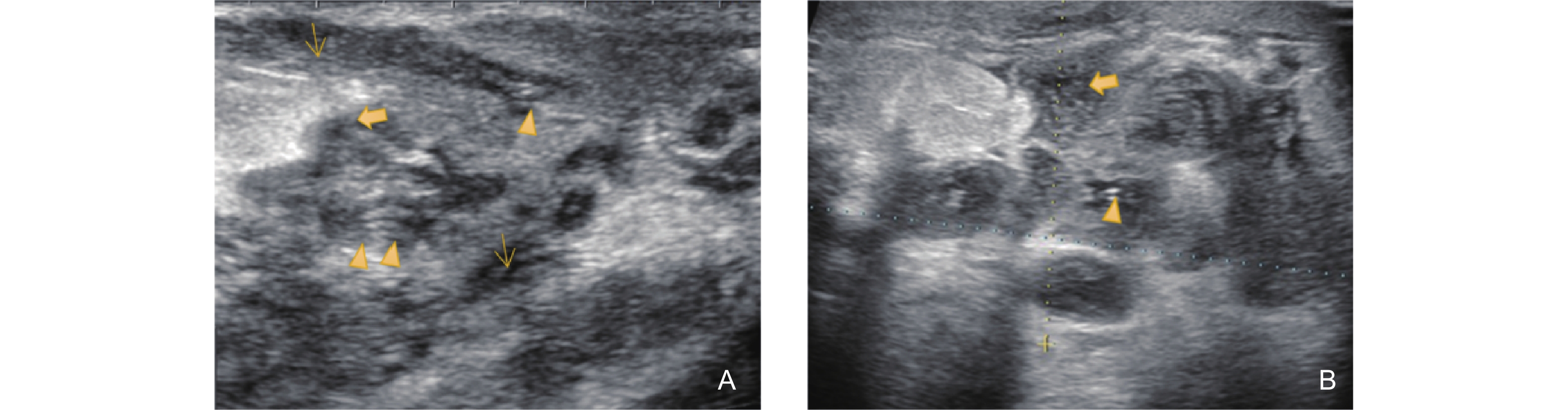
Figure 5
Ultrasonographic features of the Non-Mass Stage in GLM (type 5: coexistence of ductal inflammation, periductal Inflammation, and nodular Structures). (A) shows the sonographic appearance of several ducts behind the areola with irregular dilation. The ductal lumen is further expanded, with the inner walls thickened and rough, presenting as a ring-like high echogenicity pattern, consistent with the donut sign (triangle arrow). Two ducts merge with each other, and the surrounding ductal wall is markedly thickened, presenting as an extremely hypoechoic area (thin arrow). Another duct shows a relatively smaller diameter, with slight thickening of the ductal wall (area marked with an asterisk); (B) shows the same patient's ipsilateral breast, with a local quadrant revealing a nodular structure formed by the coexistence of dilated ducts and periductal fibrosis. Several ductal cross-sections with thickened walls are visible inside, showing high echogenicity, while the surrounding ductal area presents as hypoechoic (area marked with an asterisk)."
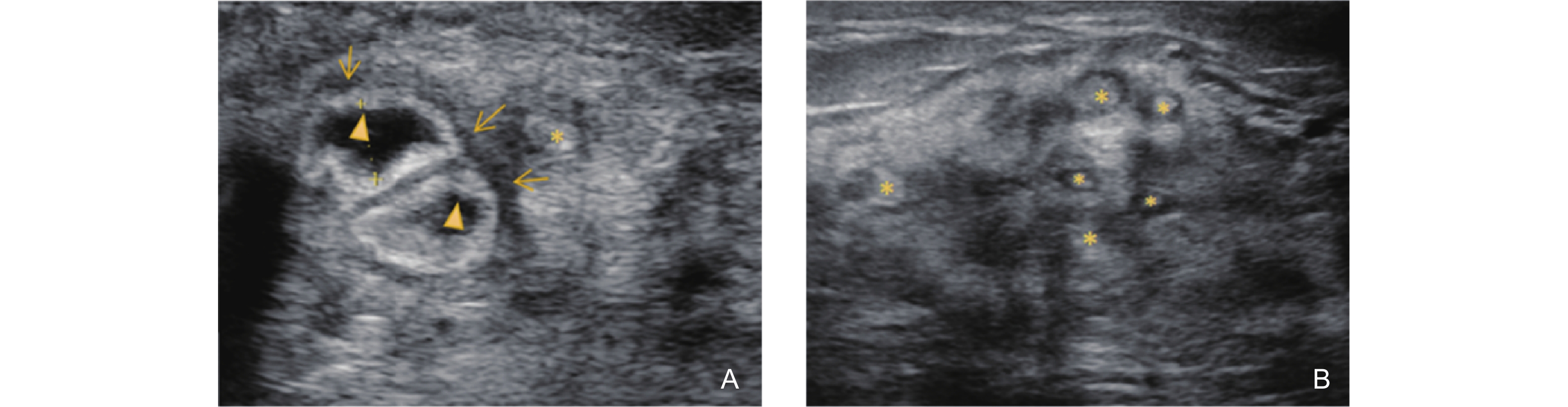
Figure 6
Ultrasonographic features of the Mass Stage in GLM. (A-B) show hypoechoic masses (M) with irregular, ill-defined margins. The masses exhibit angular extensions and a false burr sign, characterized by relatively uniform, slender hypoechoic projections radiating from the lesion edges (triangle arrows); (C) demonstrates abundant blood flow within and surrounding the mass, accompanied by skin thickening and edema in the affected area (asterisk); (D) shows thickening of Cooper’s ligaments in some cases (thin arrow)."
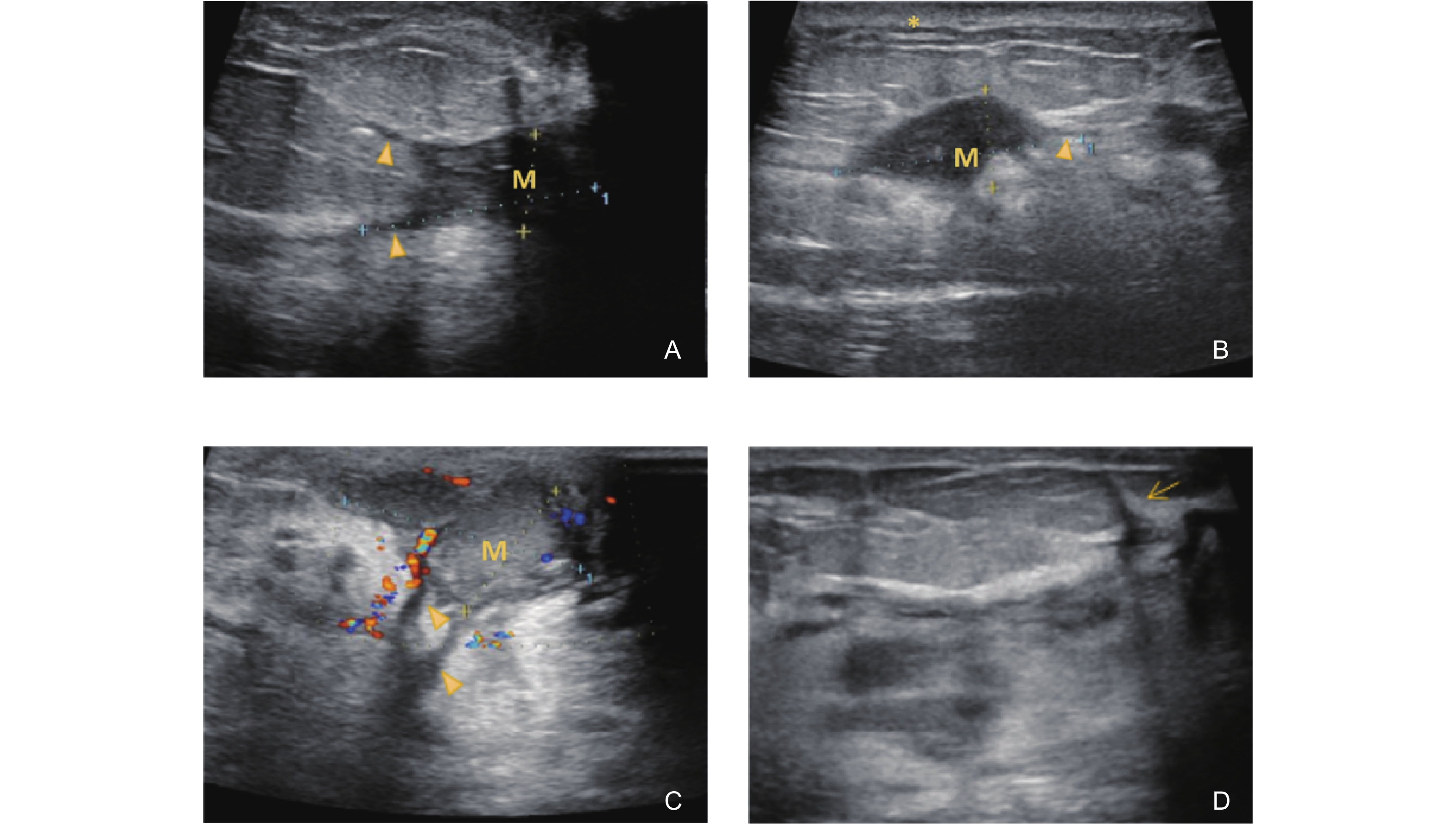
Figure 7
Ultrasonographic features of the Abscess Stage in GLM. (A-B) shows a large area of mixed echogenicity in the areolar region. The inner wall of the abscess is irregularly thickened with a rough surface (triangle arrow). Overlying skin edema and thickening are observed (asterisk). (B) shows a dilated duct extending toward the nipple is also visible (thin arrow)."
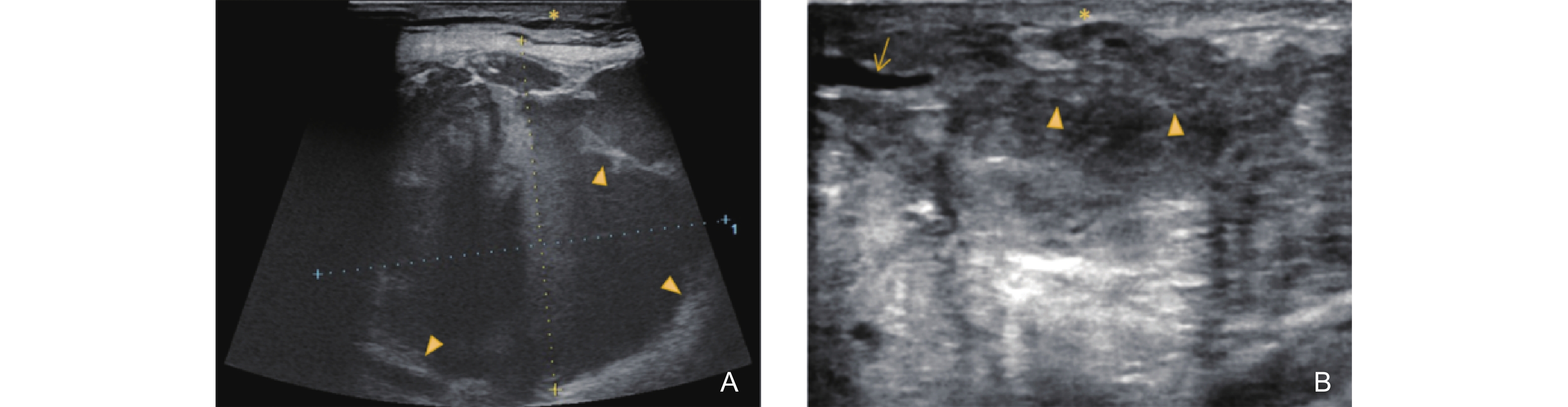
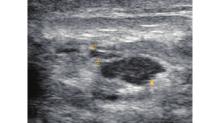
Figure 8
Ultrasonographic features of the Late Ulceration Stage in GLM. Figure 8 shows a hypoechoic area in the areolar region with relatively smooth and well-defined margins, though some portions appear blurred and irregular (triangle arrow). Surrounding this area, dilated ducts are observed communicating with the lesion and extending toward the nipple. The inner walls of the ducts are smooth, with no observable periductal thickening (thin arrow)."
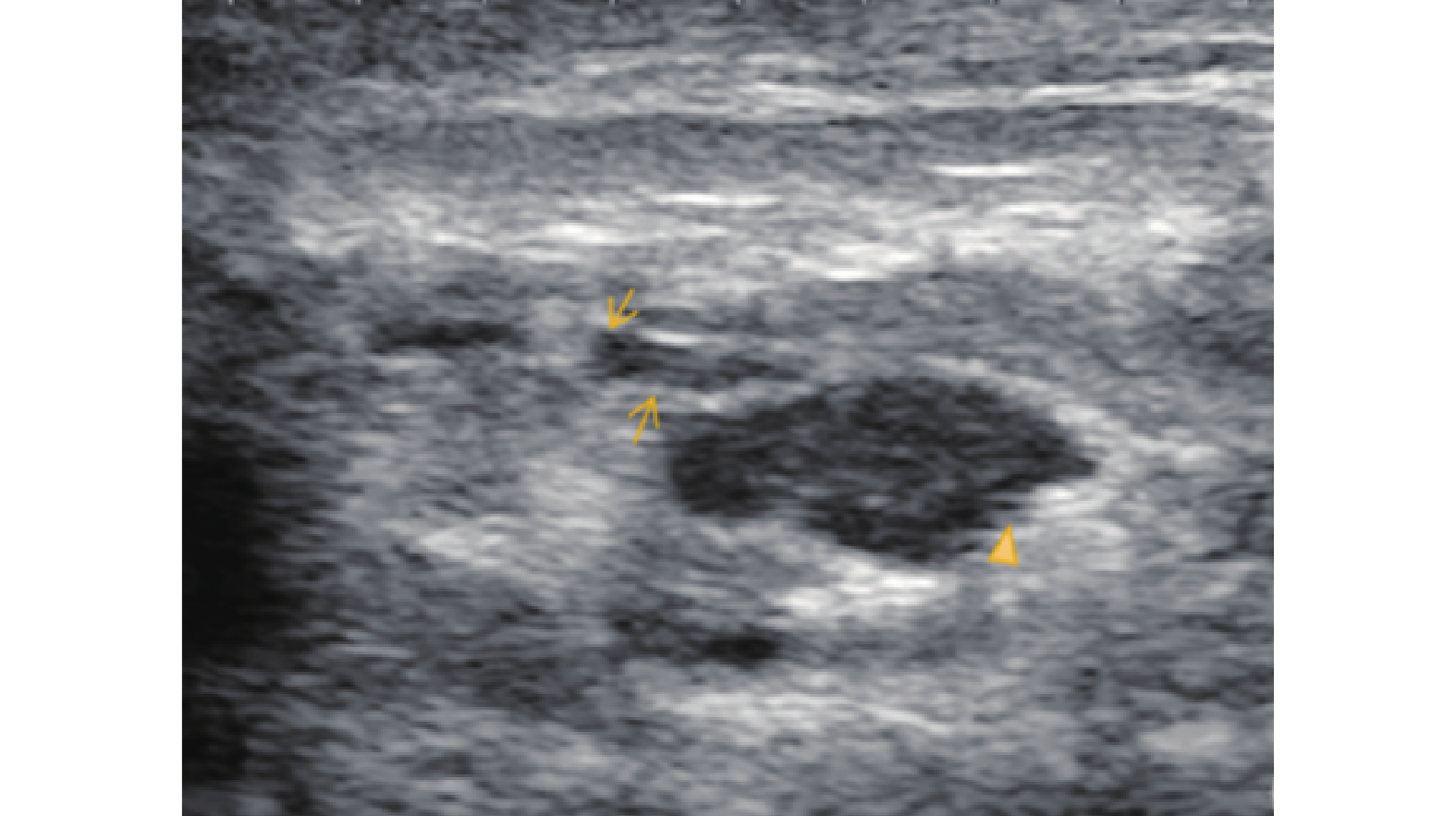

Figure 9
Ultrasonographic features of the Fistula Stage in GLM. (A) shows a duct-like hypoechoic structure beneath the nipple (N) extending toward the areolar skin. The inner wall of the duct is thickened (thin arrow), and a skin ulceration is visible at the areola (asterisk); (B) demonstrates an irregular sheet-like hypoechoic area extending from the glandular layer through the adipose tissue into the subcutaneous region, with a visible skin ulceration at the surface (asterisk)."
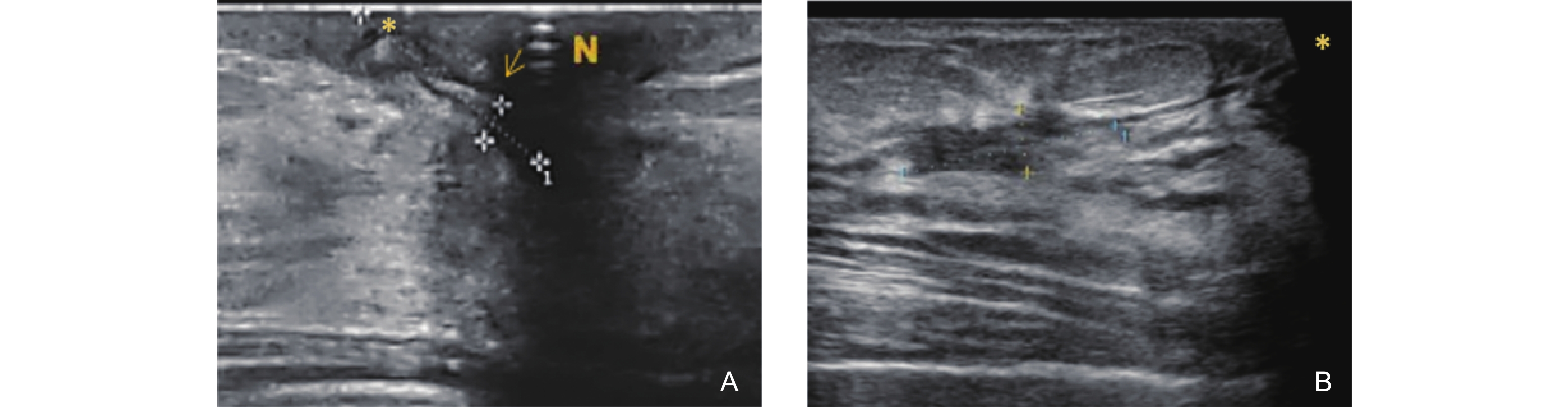
Figure 10
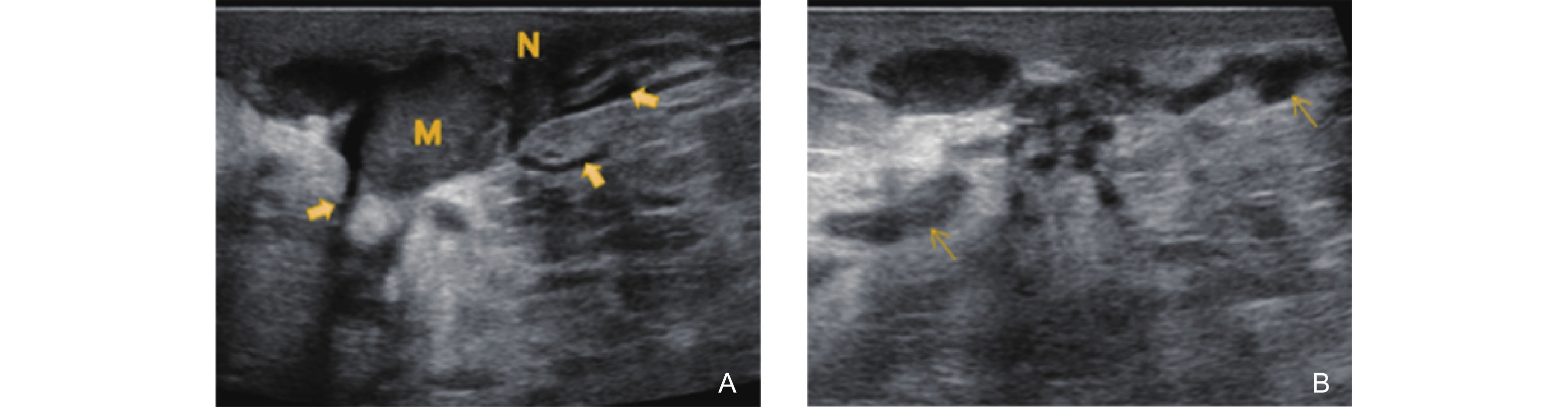
Ultrasonographic features of the Complex Type in GLM (coexistence of multiple stages). (A) shows a hypoechoic nodule located posterior to the nipple (N), with indistinct margins and angular contours. Several dilated ducts are visible surrounding the lesion (bold arrows); (B) demonstrates multiple hypoechoic ducts around the mass with luminal obliteration and thickening of both the ductal walls and surrounding tissues (thin arrows)."
| [1] | Bi J, Li Z, Lin X, Li F, Xu H, Yu X, et al. Etiology of granulomatous lobular mastitis based on metagenomic next-generation sequencing. Int J Infect Dis 2021; 113: 243-250. |
| [2] | Yuan QQ, Xiao SY, Farouk O, Du YT, Sheybani F, Tan QT, et al. Management of granulomatous lobular mastitis: an international multidisciplinary consensus (2021 edition). Mil Med Res 2022; 9: 20. |
| [3] |
Yin Y, Le H, Cheng Y, Zhong Y, Cheng Y, Wang B, et al. A cohort study of prolactin and non-puerperal mastitis using real world data. Sci Rep 2025; 15: 8619.
doi: 10.1038/s41598-025-92504-9 |
| [4] | Meng T, Cheng YQ, Qiu WQ, Ye MN, Wang B, Wu JJ, et al. Clinical study on the treatment of 120 cases of acne mastoid carbuncle with GUs’ surgery comprehensive external therapy. CJTCMP 2021; 36: 3728-3731. |
| [5] | Chen L, Zhang XY, Wang YW, Zhao QF, Ding HY. Granulomatous lobular mastitis: a clinicopathological analysis of 300 cases. Zhonghua Bing Li Xue Za Zhi 2019; 48: 231-236. |
| [6] | Alikhassi A, Azizi F, Ensani F. Imaging features of granulomatous mastitis in 36 patients with new sonographic signs. J Ultrasound 2020; 23: 61-68. |
| [7] | Dursun M, Yilmaz S, Yahyayev A, Salmaslioglu A, Yavuz E, Igci A, et al. Multimodality imaging features of idiopathic granulomatous mastitis: outcome of 12 years of experience. Radiol Med 2012; 117: 529-538. |
| [8] | Hovanessian Larsen LJ, Peyvandi B, Klipfel N, Grant E, Iyengar G. Granulomatous lobular mastitis: imaging, diagnosis, and treatment. AJR Am J Roentgenol 2009; 193: 574-581. |
| [9] | Wang M, Liu Y, Zhang D, et al. Analysis of the clinical character-istics and ultrasonographic features in 141 cases of cystic neutrophilic granulomatous mastitis. Acad Radiol 2025; 32: 2489-2496. |
| [10] | Pluguez-Turull CW, Nanyes JE, Quintero CJ, Alizai H, Mais DD, Kist KA, et al. Idiopathic granulomatous mastitis: manifestations at multimodality imaging and pitfalls. Radiographics 2018; 38: 330-356. |
| [11] | Guo JY, Yan XB, Cai ML, Lv GR. Diagnostic value of ultrasonography in different types of granulomatous lobular mastitis: a multicenter retrospective analysis of 120 cases. Fujian Med J 2022; 44: 51-54. |
| [12] | Sripathi S, Ayachit A, Bala A, Kadavigere R, Kumar S. Idiopathic granulomatous mastitis: a diagnostic dilemma for the breast radiologist. Insights Imaging 2016; 7: 523-529. |
| [13] | Villavicencio JJ, O'Brien SR, Hu T, Zuckerman S. Cystic neutrophilic granulomatous mastitis: Imaging features with histopathologic correlation. J Breast Imaging 2025; 7: 204-213. |
| [15] | Kayadibi Y, Saracoglu MS, Kurt SA, et al. Differentiation of malignancy and idiopathic granulomatous mastitis presenting as nonmass lesions on MRI: Radiological, clinical, radiomics, and clinical-radiomics models. Acad Radiol 2024; 31: 3511-3523. |
| [1] | Fu Lijia, Li Na, Liao Ziling, Lin Yanping, Li Zhaojun, Li Fan. Advances in Breast Ultrasound Segmentation and Classification [J]. Advanced Ultrasound in Diagnosis and Therapy, 2026, 10(1): 29-41. |
| [2] | Leila Bayani, MD, Donya Goodarzi, BS, Reza Mardani, MD, Bita Eslami, PhD, Sadaf Alipour, MD. Localization of Nonpalpable Breast Lumps by Ultrasound Local Coordinates and Skin Inking: A Randomized Controlled Trial [J]. Advanced Ultrasound in Diagnosis and Therapy, 2023, 7(3): 267-271. |
| [3] | Bo Jiang, MD, Yiman Du, MD, Xiang Fei, MD, Jianing Zhu, MD, Lianhua Zhu, MD, Qiuyang Li, MD, Yukun Luo, MD, PhD. Ultrasound-Guided Attenuation Parameter May Replace B-mode Ultrasound in Diagnosing Nonalcoholic Fatty Liver Disease [J]. Advanced Ultrasound in Diagnosis and Therapy, 2023, 7(3): 260-266. |
| [4] | Yi Huang, MD, Hua Wang, MD, Wenqi Cui, MD, Yujin Zong, MD, Chuyun Zheng, MD, Yue Liu, MD, Weili Min, MD, Sihan Wang, MD, Mingjun Hu, MD, Yaohui Zhang, MD. Analysis of Ultrasonic Manifestations of Pulmonary Lesions in Patients with COVID-19 [J]. Advanced Ultrasound in Diagnosis and Therapy, 2020, 4(2): 73-78. |
| Viewed | ||||||
|
Full text |
|
|||||
|
Abstract |
|
|||||
Share: WeChat
Copyright ©2018 Advanced Ultrasound in Diagnosis and Therapy
|
 Advanced Ultrasound in Diagnosis and Therapy (AUDT)
is licensed under a Creative Commons Attribution 4.0 International License.
Advanced Ultrasound in Diagnosis and Therapy (AUDT)
is licensed under a Creative Commons Attribution 4.0 International License.
