Advanced Ultrasound in Diagnosis and Therapy ›› 2024, Vol. 8 ›› Issue (4): 242-249.doi: 10.37015/AUDT.2024.240048
• Original Research • Previous Articles Next Articles
Mohammed Amra,1, Tahmasebi Aylina,1, Kim Soojib,c, Alnoury Mostafaa, E. Wessner Corinnea, Siu Xiao Taniaa, W. Gould Sharona,c, A. May Laurenb,c, Kecskemethy Heidic, T. Saul Davidc, R. Eisenbrey Johna,*( )
)
Received:2024-09-15
Accepted:2024-10-24
Online:2024-12-30
Published:2024-11-12
Contact:
R. Eisenbrey John,
E-mail:John.Eisenbrey@jefferson.edu
About author:First author contact:1 Amr Mohammed and Aylin Tahmasebi contributed equally to this study.
Mohammed Amr, Tahmasebi Aylin, Kim Sooji, Alnoury Mostafa, E. Wessner Corinne, Siu Xiao Tania, W. Gould Sharon, A. May Lauren, Kecskemethy Heidi, T. Saul David, R. Eisenbrey John. Evaluation of Liver Fibrosis on Grayscale Ultrasound in a Pediatric Population Using a Cloud-based Transfer Learning Artificial Intelligence Platform. Advanced Ultrasound in Diagnosis and Therapy, 2024, 8(4): 242-249.
Table 1
Baseline characteristics of patients and disease prevalence in the study sample"
| Patient demographics | Results |
|---|---|
| Total number of patients | 190 |
| Males | 95 |
| Females | 95 |
| Mean age | 9.3 ± 6.5 years |
| Disease distribution | Percentage (number) |
| Hepatitis | 27% (51) |
| Abnormal liver function tests | 11.5% (22) |
| MASLD/fatty liver | 20% (38) |
| Biliary conditions* | 14.7% (28) |
| Congenital/genetic conditions** | 11.1% (21) |
| Hematologic conditions*** | 1.5% (3) |
| Miscellaneous | 14% (27) |
Figure 3
(A) Shows sample ultrasound images from a biopsy-confirmed liver fibrosis case that all three radiologists misclassified as normal in all 10 images acquired, whereas AutoML accurately identified fibrosis in all 10 images; (B) Presents sample ultrasound images from a case without liver fibrosis that was correctly identified by all three radiologists in all 10 images, while AutoML consistently misclassified fibrosis in all 10 images."
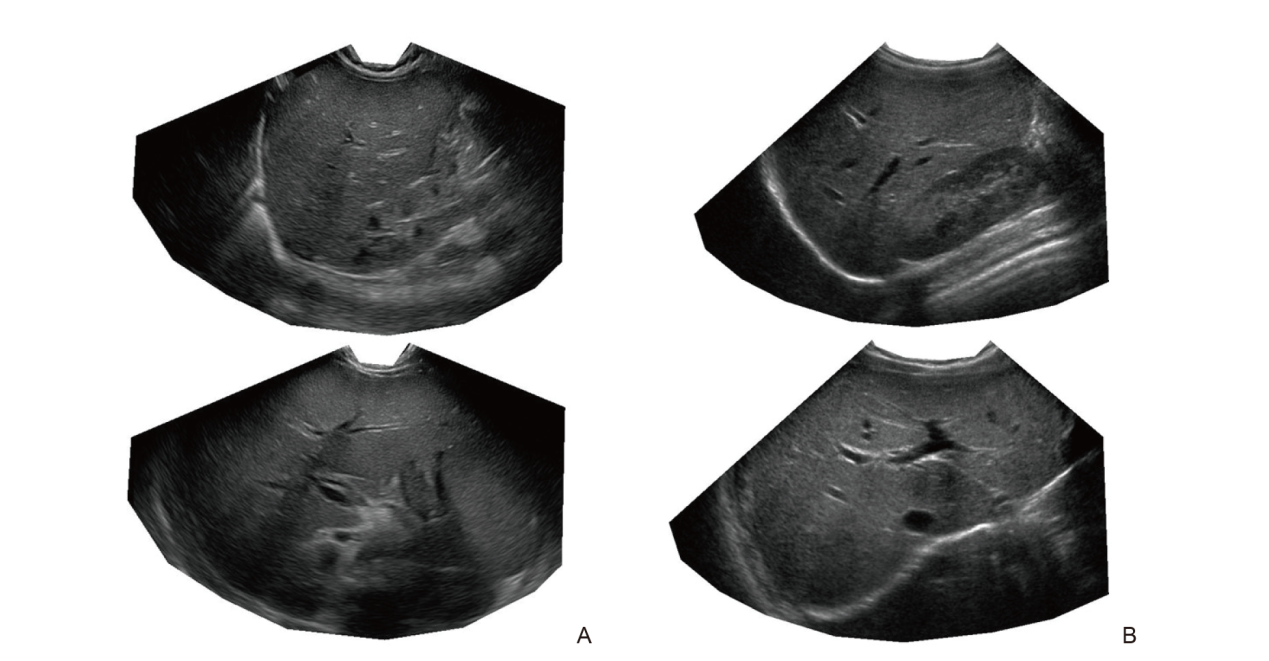
Table 3
Comparative breakdown of the diagnostic performance of the readers vs AutoML"
| Item | R1 | R2 | R3 | AutoML |
|---|---|---|---|---|
| Sensitivity [95% CI] | 46% [38% - 53%] | 39% [32% - 46%] | 40% [33% - 48%] | 70% [63% - 77%] |
| Specificity [95% CI] | 46% [39% - 54%] | 54% [46% - 61%] | 49% [41% - 56%] | 45% [37% - 52%] |
| Positive predictive value [95% CI] | 46% [41% - 51%] | 46% [40% - 52%] | 44% [38% - 50%] | 56% [52% - 60%] |
| Negative predictive value [95% CI] | 46% [41% - 51%] | 47% [42% - 51%] | 45% [40% - 50%] | 60% [53% - 66%] |
| Accuracy [95% CI] | 46% [41% - 51%] | 46% [41% - 52%] | 45% [39% - 50%] | 57% [52% - 62%] |
| Positive likelihood ratio [95% CI] | 0.86 [0.70 - 1.07] | 0.87 [0.68 - 1.10] | 0.8 [0.64 - 1.01] | 1.28 [1.09 - 1.51] |
| Negative likelihood ratio [95% CI] | 1.15 [0.94 - 1.42] | 1.11 [0.93 - 1.33] | 1.2 [0.99 - 1.45] | 0.65 [0.50 - 0.86] |
Table 4
Radiologists Inter-reader agreement in diagnosing pediatric liver fibrosis based on B-mode US images"
| Item | Observed agreements | Kappa value | SE of Kappa | 95% CI | Agreement |
|---|---|---|---|---|---|
| R1 & R2 | 314/360 (87%) | 0.74 | 0.03 | 0.67 - 0.81 | Substantial |
| R1 & R3 | 317/360 (88%) | 0.76 | 0.03 | 0.69 - 0.82 | Substantial |
| R2 & R3 | 335/360 (93%) | 0.85 | 0.02 | 0.80 - 0.91 | Almost perfect |
| [1] |
Ozdogan E, Arikan C. Liver fibrosis in children: a comprehensive review of mechanisms, diagnosis, and therapy. Clin Exp Pediatr 2022; 66:110-124.
doi: 10.3345/cep.2022.00367 pmid: 36550776 |
| [2] | Pediatric Liver Disease: Biliary Atresia & NAFLD [Internet]. 2022 [cited 2024 Jul 23]. Available from: https://liverfoundation.org/about-your-liver/facts-about-liver-disease/pediatric-liver-disease/ |
| [3] |
Lakshminarayanan B, Davenport M. Biliary atresia: A comprehensive review. J Autoimmun 2016; 73:1-9.
doi: 10.1016/j.jaut.2016.06.005 pmid: 27346637 |
| [4] |
Mărginean CO, Meliţ LE, Ghiga DV, Săsăran MO. The assessment of liver fibrosis in children with obesity on two methods: transient and two dimensional shear wave elastography. Sci Rep 2019; 9:19800.
doi: 10.1038/s41598-019-56358-2 pmid: 31875010 |
| [5] | Hunter AK, Lin HC. Review of clinical guidelines in the diagnosis of pediatric nonalcoholic fatty liver disease. Clin Liver Dis 2021; 18:40-44. |
| [6] | Sumida Y, Nakajima A, Itoh Y. Limitations of liver biopsy and non-invasive diagnostic tests for the diagnosis of nonalcoholic fatty liver disease/nonalcoholic steatohepatitis. World J Gastroenterol 2014; 20:475-485. |
| [7] |
Ovchinsky N, Moreira RK, Lefkowitch JH, Lavine JE. The liver biopsy in modern clinical practice: A pediatric point-of-view. Adv Anat Pathol 2012; 19:250-262.
doi: 10.1097/PAP.0b013e31825c6a20 pmid: 22692288 |
| [8] | Ajmera V, Loomba R. Imaging biomarkers of NAFLD, NASH and fibrosis. Mol Metab 2021; 50:101167. |
| [9] |
Nogami A, Yoneda M, Iwaki M, Kobayashi T, Kessoku T, Honda Y, et al. Diagnostic comparison of vibration-controlled transient elastography and MRI techniques in overweight and obese patients with NAFLD. Sci Rep 2022; 12:21925.
doi: 10.1038/s41598-022-25843-6 pmid: 36535977 |
| [10] |
Bonekamp S, Kamel I, Solga S, Clark J. Can imaging modalities diagnose and stage hepatic fibrosis and cirrhosis accurately? J Hepatol 2009; 50:17-35.
doi: 10.1016/j.jhep.2008.10.016 pmid: 19022517 |
| [11] |
Di Serafino M, Severino R, Gioioso M, Rossi E, Vezzali N, Pelliccia P, et al. Paediatric liver ultrasound: a pictorial essay. J Ultrasound 2020; 23:87-103.
doi: 10.1007/s40477-018-0352-z pmid: 30778891 |
| [12] | Choong CC, Venkatesh SK, Siew EPY. Accuracy of routine clinical ultrasound for staging of liver fibrosis. J Clin Imaging Sci 2012; 2:58. |
| [13] |
Mueller-Abt PR, Frawley KJ, Greer RM, Lewindon PJ. Comparison of ultrasound and biopsy findings in children with cystic fibrosis related liver disease. J Cyst Fibros 2008; 7:215-221.
pmid: 17904429 |
| [14] |
He J, Baxter SL, Xu J, Xu J, Zhou X, Zhang K. The practical implementation of artificial intelligence technologies in medicine. Nat Med 2019; 25:30-36.
doi: 10.1038/s41591-018-0307-0 pmid: 30617336 |
| [15] | Murillo Pineda MI, Siu Xiao T, Sanabria Herrera EJ, Ayala Aguilar A, Arriaga Escamilla D, Aleman Reyes AM, et al. The prediction and treatment of bleeding esophageal varices in the artificial intelligence era: A review. Cureus 2024; 16:e55786. |
| [16] | Rezazade Mehrizi MH, van Ooijen P, Homan M. Applications of artificial intelligence (AI) in diagnostic radiology: a technography study. Eur Radiol 2021; 31:1805-1811. |
| [17] | Ruan D, Shi Y, Jin L, Yang Q, Yu W, Ren H, et al. An ultrasound image‐based deep multi‐scale texture network for liver fibrosis grading in patients with chronic HBV infection. Liver Int 2021; 41:2440-2454. |
| [18] | Xue LY, Jiang ZY, Fu TT, Wang QM, Zhu YL, Dai M, et al. Transfer learning radiomics based on multimodal ultrasound imaging for staging liver fibrosis. Eur Radiol 2020; 30:2973-2983. |
| [19] | Kvostikov AV, Krylov AS, Kamalov UR. Ultrasound image texture analysis for liver fibrosis stage diagnostics. Program Comput Softw 2015; 41:273-278. |
| [20] | Sriharsha Gummadi MD. Automated machine learning in the sonographic diagnosis of non-alcoholic fatty liver disease. Adv ULTRASOUND Diagn Ther 2020; 4:176-182. |
| [21] | Wang S, Xu J, Tahmasebi A, Daniels K, Liu JB, Curry J, et al. Incorporation of a machine learning algorithm with object detection within the thyroid imaging reporting and data system improves the diagnosis of genetic risk. Front Oncol 2020; 10:591846. |
| [22] | Tahmasebi A, Qu E, Sevrukov A, Liu JB, Wang S, Lyshchik A, et al. Assessment of axillary lymph nodes for metastasis on ultrasound using artificial intelligence. Ultrason Imaging 2021; 43:329-336. |
| [23] | Tahmasebi A, Wang S, Wessner CE, Vu T, Liu JB, Forsberg F, et al. Ultrasound-based machine learning aapproach for detection of nonalcoholic fatty liver disease. J Ultrasound Med 2023; 42:1747-1756. |
| [24] | Machado P, Tahmasebi A, Fallon S, Liu JB, Dogan BE, Needleman L, et al. Characterizing sentinel lymph node status in breast cancer patients using a deep-learning model compared with radiologists’ analysis of grayscale ultrasound and lymphosonography. Ultrasound Q 2024; 40:e00683. |
| [25] | Daniels K, Gummadi S, Zhu Z, Wang S, Patel J, Swendseid B, et al. Machine learning by ultrasonography for genetic risk stratification of thyroid nodules. JAMA Otolaryngol-- Head Neck Surg 2020; 146:36-41. |
| [26] | Faes L, Liu X, Wagner SK, Fu DJ, Balaskas K, Sim DA, et al. A clinician’s guide to artificial intelligence: How to critically appraise machine learning studies. Transl Vis Sci Technol 2020; 9:7. |
| [27] | Liu Y, Chen PHC, Krause J, Peng L. How to read articles that use machine learning: Users’ guides to the medical literature. JAMA 2019; 322:1806-1816. |
| [28] |
Duan YY, Qin J, Qiu WQ, Li SY, Li C, Liu AS, et al. Performance of a generative adversarial network using ultrasound images to stage liver fibrosis and predict cirrhosis based on a deep-learning radiomics nomogram. Clin Radiol 2022; 77:e723-731.
doi: 10.1016/j.crad.2022.06.003 pmid: 35811157 |
| [29] |
Liu Z, Wen H, Zhu Z, Li Q, Liu L, Li T, et al. Diagnosis of significant liver fibrosis in patients with chronic hepatitis B using a deep learning-based data integration network. Hepatol Int 2022; 16:526-536.
doi: 10.1007/s12072-021-10294-4 pmid: 35312969 |
| [30] | Feng X, Chen X, Dong C, Liu Y, Liu Z, Ding R, et al. Multi-scale information with attention integration for classification of liver fibrosis in B-mode US image. Comput Methods Programs Biomed 2022; 215:106598. |
| [31] | Lee JH, Joo I, Kang TW, Paik YH, Sinn DH, Ha SY, et al. Deep learning with ultrasonography: automated classification of liver fibrosis using a deep convolutional neural network. Eur Radiol 2020; 30:1264-1273. |
| [32] | Al-Hasani M, Sultan LR, Sagreiya H, Cary TW, Karmacharya MB, Sehgal CM. Ultrasound radiomics for the detection of early-stage liver fibrosis. Diagnostics 2022; 12:2737. |
| [33] | Cheng HY, Wang HY, Chang WH, Lin SC, Chu CH, Wang TE, et al. Nonalcoholic fatty liver disease: Prevalence, influence on age and sex, and relationship with metabolic syndrome and insulin resistance. Int J Gerontol 2013; 7:194-198. |
| [34] | Heyens LJM, Busschots D, Koek GH, Robaeys G, Francque S. Liver fibrosis in non-alcoholic fatty liver disease: From liver biopsy to non-invasive biomarkers in diagnosis and treatment. Front Med 2021; 8:615978. |
| [35] | Krishnan G, Singh S, Pathania M, Gosavi S, Abhishek S, Parchani A, et al. Artificial intelligence in clinical medicine: catalyzing a sustainable global healthcare paradigm. Front Artif Intell 2023; 6:1227091. |
| [36] | Das A, Connell M, Khetarpal S. Digital image analysis of ultrasound images using machine learning to diagnose pediatric nonalcoholic fatty liver disease. Clin Imaging 2021; 77:62-68. |
| [37] |
Zhou W, Yang Y, Yu C, Liu J, Duan X, Weng Z, et al. Ensembled deep learning model outperforms human experts in diagnosing biliary atresia from sonographic gallbladder images. Nat Commun 2021; 12:1259.
doi: 10.1038/s41467-021-21466-z pmid: 33627641 |
| [38] | Hsu FR, Dai ST, Chou CM, Huang SY. The application of artificial intelligence to support biliary atresia screening by ultrasound images: A study based on deep learning models. PLOS ONE 2022; 17:e0276278. |
| [1] | Liu Taixia, Wang Hanxiang, Wang Dan, Zhang Yuke, Guo Yunyun, Liu Shuo, Zhang Minfeng, Nie Hongming, Shen Rui. The Role of Sonazoid-contrast-enhanced Ultrasound In Precision Diagnosis and Guidance for Radiofrequency Ablation Therapy of Hepatocellular Carcinoma: a Literature Review [J]. Advanced Ultrasound in Diagnosis and Therapy, 2026, 10(1): 20-28. |
| [2] | Fu Lijia, Li Na, Liao Ziling, Lin Yanping, Li Zhaojun, Li Fan. Advances in Breast Ultrasound Segmentation and Classification [J]. Advanced Ultrasound in Diagnosis and Therapy, 2026, 10(1): 29-41. |
| [3] | Li Na, Li Fan. Focused Ultrasound Combined with Microbubbles for Inducing Blood-Brain Barrier Opening: Cavitation Monitoring and Control [J]. Advanced Ultrasound in Diagnosis and Therapy, 2026, 10(1): 51-58. |
| [4] | Yin Yulian, Cheng Yifan, Zhou Liangmei, Zhong Yuanyuan, Wang Bing, Wu Jingjing, Ren Yajuan, Gao Dongwen, Chen Hongfeng, Ye Meina, Yin Haoqiang. From Non-Mass Stage to Complex Type: Ultrasonographic Assessment of Granulomatous Lobular Mastitis Across Six Clinical Stages [J]. Advanced Ultrasound in Diagnosis and Therapy, 2026, 10(1): 59-68. |
| [5] | Syahril Erlin, Abdullah Nusratuddin, Ilyas Muhammad, As’ad Suryani, Choridah Lina, Natzir Rosdiana, Kurniawan Liong Boy, Bahar Burhanuddin, Mappaware Nasrudin A., Mulyadi Farah Ekawati, Yacca Susdiaman Sudin. The Effects of Ajwa Dates Consumption (Phoenix dactylifera L), on Ovarian Follicular Features with Transvaginal Ultrasound in Perimenopausal Women [J]. Advanced Ultrasound in Diagnosis and Therapy, 2026, 10(1): 69-73. |
| [6] | Si Jiahao, Zhang Ye, Wang Shuaiyanga, Hao Liuwei, Duan Shaobo. Ultrasound-Guided Portal Vein Puncture for The Treatment of Hepatic Portal Venous Gas: A Case Report [J]. Advanced Ultrasound in Diagnosis and Therapy, 2026, 10(1): 74-78. |
| [7] | Guan Xin, Hu Xinyuan, Han Hong, Zhang Dezhi, Xu Huixiong. The Evolving Application of Ultrasound in the Precision Management of Small Hepatocellular Carcinoma [J]. Advanced Ultrasound in Diagnosis and Therapy, 2025, 9(4): 375-387. |
| [8] | Li Yanran, Cui Yuanjie, Wu Qingqing, Zhang Na. Current Applications of Artificial Intelligence in Obstetric Ultrasound [J]. Advanced Ultrasound in Diagnosis and Therapy, 2025, 9(4): 449-456. |
| [9] | Hou Wenfei, Chen Wanting, Liu Huazhen, Tang Jiajia, Yang Meng. Applications of Ultrasound Localization Microscopy in Abdominal Imaging [J]. Advanced Ultrasound in Diagnosis and Therapy, 2025, 9(4): 347-356. |
| [10] | Yu Xiao jie, Song Zheng lai, Chang Xue yong, Yu Jie, Liang Ping. Artificial Intelligence in Ultrasound Diagnosis of Liver Nodules: A Comprehensive Review of B-Mode and Contrast-enhanced Applications [J]. Advanced Ultrasound in Diagnosis and Therapy, 2025, 9(4): 326-346. |
| [11] | Zhong Xian, Xie Xiaoyan. Multimodal Ultrasound Radiomics in Liver Disease: Current Status and Future Directions [J]. Advanced Ultrasound in Diagnosis and Therapy, 2025, 9(4): 388-408. |
| [12] | Zhang Xiaoqian, Zhang Jingwen, Dong Yijie, Zhou Jianqiao. Research Progress and Clinical Translation of Photoacoustic–ultrasound Fusion Imaging in Breast Cancer Diagnosis and Therapy [J]. Advanced Ultrasound in Diagnosis and Therapy, 2025, 9(4): 467-482. |
| [13] | Jin Tong, Yu Xiaohu, Ai Zheng, Guo Hongcheng. Artificial Intelligence in Ultrasound Imaging: A Review of Progress from Machine Learning to Large Language Model [J]. Advanced Ultrasound in Diagnosis and Therapy, 2025, 9(4): 483-496. |
| [14] | Xiang Xi, Yang Yujia, Wang Liyun, Qiu Li. Advances and Applications in Dermatological Ultrasound [J]. Advanced Ultrasound in Diagnosis and Therapy, 2025, 9(4): 457-466. |
| [15] | Zheng Hairong, Meng Long, Li Fei, Niu Lili, Qiu Weibao, Ma Teng, Liu Chengbo, Zhu Xuefeng, Wan Liwen, Cai Feiyan. Advance in Ultrasound Super-resolution Imaging, Cell Manipulation and Inter-brain Communication [J]. Advanced Ultrasound in Diagnosis and Therapy, 2025, 9(4): 307-325. |
| Viewed | ||||||
|
Full text |
|
|||||
|
Abstract |
|
|||||
Share: WeChat
Copyright ©2018 Advanced Ultrasound in Diagnosis and Therapy
|
 Advanced Ultrasound in Diagnosis and Therapy (AUDT)
is licensed under a Creative Commons Attribution 4.0 International License.
Advanced Ultrasound in Diagnosis and Therapy (AUDT)
is licensed under a Creative Commons Attribution 4.0 International License.
